Hurricane Idalia looms over florida
As Hurricane Idalia intensified moves through Florida and up the U.S. coast, residents are on high alert.
Tropical Storm Idalia rapidly transformed into a Category 3 hurricane. Life-threatening storm surges and dangerous winds have swept through various parts of Florida and forecasters predict it will continue up the coast.
West Virginia suffers from unrelenting flooding
As Florida prepared for Hurricane Idalia, West Virginia grappled with the aftermath of excessive rainfall, leading to widespread flooding. Gov. Jim Justice declared a State of Emergency for Kanawha, Braxton, Calhoun, Clay, and Roane counties. The torrential rains have inflicted damage upon homes, bridges, and roads in these regions.
Gov. Justice’s statement can be found here.
Ensuring food safety amidst the chaos
With both regions facing unique challenges, ensuring food safety during and after these catastrophic events remains a top priority. The U.S. Food and Drug Administration and other organizations provide crucial guidelines for residents to safeguard their food and health.
Before a storm hits:
- Elevate refrigerators and freezers off the ground using cement blocks.
- Move canned goods and foods from basements or low cabinets to higher areas.
Food safety after flooding:
- Use bottled drinking water that hasn’t come into contact with floodwater.
- Discard any food that may have been exposed to floodwater, particularly if not in waterproof containers.
- Inspect canned foods for damage, and discard damaged cans.
- Thoroughly wash and sanitize metal pans, dishes, and utensils using a chlorine bleach solution.
During power outages:
- Keep refrigerator and freezer doors closed to maintain safe temperatures.
- Use ice packs, coolers, and frozen containers of water or gel packs to preserve food freshness.
After power restoration:
- Check refrigerator and freezer temperatures; follow guidelines for safe food storage.
- Discard perishable foods that have been at temperatures above 40 degrees F for 4 hours or more.
- Refreeze frozen food if temperature remains at 40 degrees F or below.
Farmers’ concerns and resources:
- For farmers, these weather events pose serious risks to their crops. The FDA provides guidance on assessing potential damage to food crops affected by floods. If edible portions of crops are exposed to contaminated floodwaters, they’re considered adulterated and unsuitable for human consumption. Farmers are advised to evaluate the safety of crops on a case-by-case basis for potential food safety concerns.
Both West Virginia and Florida are currently marshaling resources, emergency teams, and relief efforts to aid affected residents. By following these essential food safety tips, individuals can better protect themselves and their families during these trying times. For more information, residents can access resources provided by local health departments and relevant agencies, or contact the USDA Meat and Poultry Hotline at 888-MPHotline.
Stay safe, stay informed, and stay prepared as these natural disasters unfold.
(To sign up for a free subscription to Food Safety News, click here.)
]]>1. Weekly Menu Planning and Grocery Shopping
The process, as easy as 1, 2, 3, 4, begins with Weekly Menu Planning and Grocery Shopping. Parents are advised to plan their children’s lunch menus for the week ahead, researching ideas online and crafting a comprehensive shopping list. While shopping, a vital tip is to place frozen or refrigerated items in the cart last, just before reaching the cashier, to ensure they stay cold longer. Preventing cross-contamination is also emphasized, with a reminder to keep raw meat and poultry separate from other groceries and considering the use of bags to contain any potential leakage. Furthermore, perishable items must be stored in the fridge or freezer within two hours of purchase.
2. Safe Food Preparation
The second step, Safe Food Preparation, underlines the importance of thorough handwashing, an elementary yet frequently neglected practice. A recent USDA study has highlighted that 97 percent of participants failed to wash their hands correctly or at all when required. Proper hand hygiene is paramount to prevent foodborne illnesses, which can be transmitted through contaminated hands. The rule is clear: wash hands with soap and warm water for a full 20 seconds and dry them with a clean towel. Ensuring clean utensils, countertops, and cutting boards is equally imperative. Once these hygiene steps are observed, parents can proceed to prepare lunches for the week, including ready-to-eat items and boiled eggs.
3. Safe Packing
Safe Packing constitutes the third step and emphasizes the role of temperature control in maintaining food safety. Packing perishable items in an insulated lunch bag is recommended, as paper bags do not provide adequate insulation. To ensure optimal coldness, storing the insulated bag in the freezer overnight is advised. Two cold sources, such as frozen water bottles or freezer packs, are recommended to maintain temperatures below 40 degrees F until lunchtime. Hot items should be packed in insulated containers, which should be preheated with boiling water before the food is placed inside.
4. Safe Cooking
Lastly, the fourth step of Safe Cooking requires the use of food thermometers when preparing meals that require cooking, such as frozen foods. Food thermometers are essential to verify that the internal temperature of the food reaches safe levels to eliminate harmful bacteria. Different foods have different safe internal temperatures, and following manufacturer cooking instructions on frozen foods is equally crucial.
Sandra Eskin, Deputy Under Secretary for Food Safety at the U.S. Department of Agriculture (USDA), stresses the importance of prioritizing food safety during back-to-school preparations. “Because children are particularly at risk for serious foodborne illness, food safety must be at the top of the list when preparing lunches for school and field trips,” says Eskin.
By adhering to the four-step approach of meal preparation, parents can enjoy the peace of mind that comes with knowing their children’s lunches are both nutritious and secure.
(To sign up for a free subscription to Food Safety News, click here.)
]]>The USDA has some tips for parents and caregivers to help them make the food safety honor roll.
Keep Cold Foods Cold and Hot Foods Hot
- Cold Foods: USDA recommends using insulated lunch boxes to keep food safe. Paper bags are risky because they don’t allow for proper food cooling. Always use at least two cold sources, like frozen gel packs, juice boxes, or water bottles, to keep foods cold. Foods that sit out at room temperature risk entering the “Danger Zone” (temperatures between 40 degrees F and 140 degrees F, where bacteria can multiply quickly and cause illness).
- Hot Foods: When packing hot foods like chili, soups, or stews, use an insulated container to keep the food hot. Keep the container closed until lunchtime to keep the food at 140 degrees F or above.
If preparing lunch the night before school and refrigerating overnight, take the bag or lunchbox out just before leaving home. Pack just the amount of perishable food that can be eaten at lunchtime. That way, there won’t be a problem with the storage or safety of leftovers.
Remember the Four Steps to the Food Safety Honor Roll
Clean—Wash hands with soapy water for 20 seconds before touching food.
Separate—Keep raw meats separate from ready-to-eat food.
Chill—Refrigerate foods promptly. Discard foods left at room temperature for over 2 hours.
Cook—Use a food thermometer to know your meat and poultry are fully cooked to a safe internal temperature.
For more information, call the USDA Meat and Poultry Hotline at 1-888-MPHotline (1-888-674-6854) or email [email protected] to reach a food safety specialist or chat live at ask.usda.gov from 10 a.m. to 6 p.m. Eastern Time, Monday through Friday.
(To sign up for a free subscription to Food Safety News, click here.)
]]>However, a number of outbreaks of foodborne illness from eating raw or undercooked fiddleheads have been reported in the United States and Canada since 1994. Proper handling and thorough cooking of fiddleheads can reduce the risk of foodborne illness.
Tips for safe consumption of fiddleheads:
Cleaning Fresh Fiddleheads
Before cooking fiddleheads, it is important to clean them properly. To do this, remove as much of the brown papery husk as possible using your fingers. Then, wash the fiddleheads in fresh, cold water to remove any residual husk or dirt.
Cooking Fiddleheads
Under no circumstances should fiddleheads be eaten raw. To ensure they are safe for consumption, follow these steps:
- Cook them in a generous amount of boiling water for 15 minutes or steam them for 10 to 12 minutes.
- Discard the water used for boiling or steaming fiddleheads and thoroughly wash pans and bowls used for cooking.
- Follow the above instructions before sautéing, frying, baking, or making other foods (e.g. soups, casseroles) using fiddleheads.
Freezing Fiddleheads
If you plan to freeze fiddleheads, it is important to follow these steps:
- Clean fiddleheads as outlined above.
- Blanch fiddleheads for two minutes.
- Plunge fiddleheads in cold water. Drain.
- Discard the blanching water.
- Pack drained fiddleheads in freezer containers or bags.
- Store them in the freezer for up to one year.
- Follow the complete cooking steps outlined above before.
(To sign up for a free subscription to Food Safety News, click here)
]]>The steps are to keep clean; avoid contamination; keep food products safe; reduce contact with animals; and stay safe and protect yourself. They are based on the five keys for safer food which are to keep clean; separate raw and cooked food; cook thoroughly; keep food at safe temperatures; and use safe water and raw materials.
WHO is calling on authorities in member states to strengthen their regulatory basis to improve hygiene and sanitation standards in traditional markets. Such actions can reduce the risks of transmission and spread of zoonotic, foodborne, and emerging infectious diseases.
Potential problems
Traditional food markets, including wet and informal markets, differ from country to country but are common in the Asia Pacific. These markets play an important economic, cultural, and social role and are sources of livelihood for millions of people in urban and rural areas. Items sold include vegetables, fruits, dairy products, spices, fresh meat, fish and other seafood.
However, when not managed properly, they can be unsafe environments that pose serious health risks. The mixture of humans and animals, poor hygiene conditions, and the proximity of foods of animal and plant origin can create favorable conditions for the spread of diseases and entry points for contaminants, said WHO.
Drawbacks related to market infrastructure, poor access and provision of basic sanitation services, and inadequate cleaning are the main obstacles to maintaining food safety along the supply chain. Other issues include food handling, cross-contamination, and temperature control.
Enforcement of good practices is often a challenge as food inspectors are not always adequately trained plus inspection protocols and traceability systems, especially for meat products, are often weak or nonexistent. Many traditional markets are also at risk of flooding due to heavy rainfall.
The document provides guidance on the implementation of the five keys for safer food markets to guide market managers.
WHO regional offices in the Western Pacific and South-East Asia contributed to the work. Feedback was gathered from attendees at a meeting on risk mitigation in traditional food markets in September 2021 in Manila, Philippines.
Examples under the five points
As part of the keep clean point, WHO said to reduce the level of contaminants in the market, closure to perform deep cleaning and disinfection of all areas, equipment, and utensils needs to take place at least every two weeks. Attention must also be paid to waste disposal.
The second avoids contamination key suggests having a zoning system with separate areas for stalls selling raw food like meat, fish, and poultry from vegetables, dry food, and ready-to-eat foods. A different space should be used to sell live animals.
The third area advises using only products from reliable suppliers that are within their shelf life, with processed foods having clear labels and intact packaging. Chemicals should be stored away from food.
The fourth key covers pest control programs, animal health, and welfare. The final topic looks at preventing human-to-human transmission of diseases.
In related work, a WHO group on traditional food markets is meeting virtually from June 13 to 15. Experts will try to agree on the scope, key questions for developing guidelines to transform these markets, and definition of the work plan.
(To sign up for a free subscription to Food Safety News, click here.)
]]>The group has compiled its list for several years to highlight produce with pesticide residues. All of the fresh fruits and vegetables on the list have residues below the legal limits but are culled from a list of thousands of tests by the USDA.
This year the Environmental Working Group, EWG, says a single strawberry tested positive for 22 different pesticides. The EWG suggests that consumers buy organic fruits and vegetables to avoid such situations. Some pesticides are approved for use on organic crops.
“Strawberries aren’t the only problematic produce item. 90 percent of blueberry samples were contaminated with toxic pesticide residues, including pesticides linked to cancer and nervous system harm,” according to the EWG.
“Among the 54 pesticides found on blueberries were several bee-killing neonic pesticides. Not only have these pesticides been linked to the massive decline in bee populations worldwide, they’ve also been linked to neurological damage in children.”
The organization says 75 percent of non-organic fruits and vegetables sold in the U.S. are “riddled” with potentially toxic agricultural chemicals. Some of the pesticides detected have been banned in the U.S. or Europe because of concerns about how they harm people.
“Despite the abundance of science linking exposure to pesticides with serious health issues, a potentially toxic cocktail of concerning chemicals continues to taint many of the non-organic fruits and vegetables are eaten by consumers,” said Alexis Temkin, EWG toxicologist.
EWG’s analysis of the latest fruit and vegetable is from testing data from the U.S. Department of Agriculture and the U.S. Food and Drug Administration. The 2023 edition includes data from 46,569 samples of 46 fruits and vegetables, covering 251 different pesticides.
“Everyone – adults and kids – should eat more fruits and vegetables, whether organic or not,“ Temkin said. “A produce-rich diet provides many health benefits.
“But in the ongoing absence of meaningful federal oversight, consumers concerned about pesticide exposure can use EWG’s Shopper’s Guide to Pesticides in Produce to navigate the produce aisle in ways that work best for them and their families.”
The fruits and vegetables on EWG’s Dirty Dozen for this year are:
1. Strawberries
2. Spinach
3. Kale, collard, and mustard greens
4. Peaches
5. Pears
6. Nectarines
7. Apples
8. Grapes
9. Bell and hot Peppers
10. Cherries
11. Blueberries
12. Green Beans
The group also compiles a list of what it considers to be the cleanest produce in terms of pesticide residues. This year the Clean 15 are:
1. Avocados
2. Sweet corn*
3. Pineapple
4. Onions
5. Papaya*
6. Sweet peas (frozen)
7. Asparagus
8. Honeydew melon
9. Kiwi
10. Cabbage
11. Mushrooms
12. Mangoes
13. Sweet Potatoes
14. Watermelon
15. Carrots
* Some sweet corn, papaya, and summer squash sold in the United States is produced from genetically modified seeds. The EWG recommends that consumers buy organic varieties of these crops if they want to avoid genetically modified produce.
(To sign up for a free subscription to Food Safety News ,click here)
]]>The Food and Drug Administration says the Food Code is the agency’s “best advice for a uniform system of provisions that address the safety and protection of food offered at retail and in food service.”
The 2022 edition is now available for adoption by local, state, and federal governmental jurisdictions for administration by the various departments, agencies, bureaus, divisions, and other units within each jurisdiction that have been delegated compliance responsibilities for food service, retail food stores, or food vending operations.
Alternatives that offer an equivalent level of public health protection to ensure that food at retail and food service is safe are recognized by the 2022 Food Code. It reflects the agency’s continued commitment to maintaining cooperative programs with state, local, tribal, and territorial governments, according to FDA.
The 2022 edition reflects the input of regulatory officials, industry, academia, and consumers that participated in the 2020 biennial meeting of the Conference for Food Protection (CFP), which was held in 2021.
The FDA encourages its state, local, tribal, and territorial partners to adopt the latest version of the FDA Food Code. The benefits associated with the complete and widespread adoption of the 2022 Food Code as statutes, codes, and ordinances include:
- Reduction of the risk of foodborne illnesses within food establishments, thus protecting consumers and industry from potentially devastating health consequences and financial losses.
- Uniform standards for retail food safety reduce complexity and better ensure compliance.
- The elimination of redundant processes for establishing food safety criteria.
- The establishment of a more standardized approach to inspections and audits of food establishments.
Members of the FDA’s National Retail Food Team are available to assist regulatory officials, educators, and the industry in their efforts to adopt, implement, and understand the provisions of the FDA Food Code and the Retail Program Standards. Inquiries may be sent to [email protected] or directly to a Retail Food Specialist located in one of the FDA’s three Retail Food Protection Branches across the country.
Food Code 2022 (PDF: 4.68MB)
Summary of Changes in the 2022 FDA Food Code
(To sign up for a free subscription to Food Safety News, click here.)
]]>Food needs to be stored properly so it can be enjoyed for a couple more days.
To ensure that your holiday spread remains safe to eat, follow these guidelines:
- Two-hour rule: All perishable items should be refrigerated within two hours of coming out of the oven or refrigerator. After two hours, perishable food enters the Danger Zone — between 40 degrees F to 140 degrees F — where bacteria can multiply quickly and cause the food to become unsafe. If foods have been left out for more than two hours, discard items to prevent foodborne illness. The two-hour rule includes “doggie bags” sent home with guests.
- Use small and shallow containers: Store leftover food in small, shallow containers in the refrigerator or in the freezer for later use. Shallow containers help cool leftovers more quickly than storing them in large containers.
- Freeze or consume within four days: If you want to keep leftovers longer than four days, freeze them within that period. Food poisoning bacteria — except for Listeria and hepatitis A — do not grow in the freezer. Foods that have been in the freezer for months (recommended freezer times chart) may be dry, or may not taste as good. If you store leftovers in the freezer, the quality will be best within two to six months. Reheat leftovers to an internal temperature of 165 degrees F.
Reheating
- When reheating in the microwave, cover and rotate the food for even heating. Arrange food items evenly in a covered microwave-safe glass or ceramic dish and add some liquid if needed. Because microwaves have cold spots, check the internal temperature of the food in several places with a food thermometer after allowing a resting time.
- Reheat sauces, soups, and gravies by bringing them to a rolling boil.
- Do not use slow cookers for reheating.
- Leftovers are safe to eat once they have reached an internal temperature of 165 degrees F.
- If you decide to freeze your leftovers, use the Safe Defrosting Methods when you want to reheat.
Curious about how long a specific food will last in the fridge or freezer? Check out this helpful chart from the FDA.
(To sign up for a free subscription to Food Safety News, click here.)
]]>Here are four simple rules to keep your family safe this holiday season — clean, separate, cook and chill.

“Clean” reminds consumers to wash their hands and kitchen surfaces often during cooking. “Separate” prevents cross-contamination by encouraging consumers to keep their raw meats away from other foods. “Cook” informs consumers of the necessity of cooking their meat, poultry, fish and egg products to the right internal temperature. “Chill” highlights the importance of prompt refrigeration of food. Focusing on those behaviors provides consumers with clear steps they can take to protect themselves and their families from food poisoning.
Are you a Christmas ham or turkey family?
Ham cooking safety tips from the USDA:
- Both whole or half, cooked, vacuum-packaged hams packaged in federally inspected plants and canned hams can be eaten cold, right out of the package.
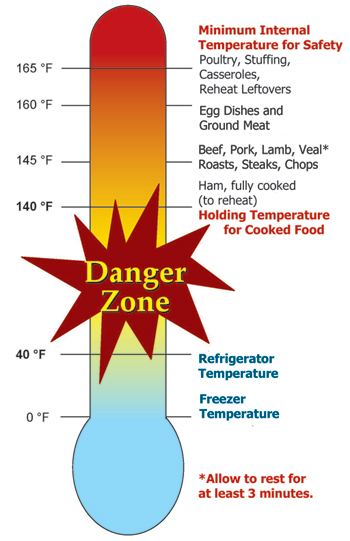
- If you want to reheat these cooked hams, set the oven no lower than 325 degrees F and heat the meat to an internal temperature of 140 degrees F as measured with a food thermometer.
- Unpackaged, cooked ham is potentially contaminated with pathogens. For cooked hams that have been repackaged in any other location outside the processing plant or for leftover cooked ham, heat to 165 degrees F.
- Spiral-cut cooked hams are also safe to eat cold, if they have been held at proper temperatures. These hams are best served cold because heating sliced whole or half hams can dry out the meat and cause the glaze to melt and run off the meat. If reheating is desired, hams that were packaged in processing plants under USDA inspection must be heated to 140 degrees F as measured with a food thermometer (165 degrees F for leftover spiral-cut hams or ham that has been repackaged in any other location outside the plant). To reheat a spiral-sliced ham in a conventional oven, cover the entire ham, or individual portions, with heavy aluminum foil and heat at 325 degrees F for about 10 minutes per pound. Individual slices may also be warmed in a skillet or microwave, but must reach 165 degrees F.
- Cook-before-eating hams or fresh hams must reach 145 degrees F (with a 3-minute rest time) to be safely cooked before serving. Cook in an oven set no lower than 325 degrees F. Hams can also be safely cooked in a microwave oven, other countertop appliances, and on the stove. Consult a cookbook for specific methods and timing.
- Country hams can be soaked for 4 to 12 hours or longer in the refrigerator to reduce the salt content before cooking. Then they can be cooked by boiling or baking. Follow the manufacturer’s cooking instructions.
Turkey cooking safety tips from the USDA:
Thaw the turkey safely

Perishable foods should never be thawed on the counter, at room temperature or in hot water. They must not be left at room temperature for more than two hours. There are safe ways to thaw a turkey and other food, including in the refrigerator, in cold water and in the microwave.
Even though the center of the food may still be frozen as it thaws on the counter, the outer layer of the food can easily be in the “Danger Zone,” between 40 degrees F and 140 degrees F. The danger zone allows potentially deadly bacteria to multiply rapidly.
Remove the giblets from the turkey cavities after thawing and cook them separately.
Thoroughly cook your turkey
- Use a meat thermometer to determine when the turkey is done. The turkey is done when the thermometer reaches 165 degrees Fahrenheit.
- Insert the thermometer in the thickest part of the turkey thigh. Be aware dark meat takes longer to cook than any other part.
- Basting the turkey while it is cooking is not necessary. Basting tools could be sources of bacterial contamination if dipped into uncooked or undercooked poultry juices and then allowed to sit at room temperature for later basting. Washing tools between bastings can help reduce pathogens.
- Do not cook a turkey overnight in an oven set at a low temperature. Cooking a turkey at a temperature below 325 degrees Fahrenheit allows harmful bacteria to multiply.
- If you purchase a fully cooked turkey, pick it up hot and take it home to eat immediately or refrigerate it.
Holiday specials
- If your eggnog is egg-based make sure to cook the base to a minimum safe temperature of 160 degrees F. Adding alcohol does not make eggnog safe for consumption.
- “Tiger meat” or “cannibal sandwiches” are a winter holiday dish common in the upper Midwest as well as other parts of the country. It contains raw ground meat, usually beef, seasoned with spices and onion and sometimes raw eggs, and served on bread or a cracker. Hundreds are sickened every year from eating this dish. Never eat raw meat. Both ground beef and raw eggs pose health hazards when eaten undercooked or raw. A safe alternative is to mix ground beef with spices and onion and cook it to a safe 160 degrees F.
- When baking this holiday season do not eat raw dough if it contains eggs or unbaked flour.
(To sign up for a free subscription to Food Safety News, click here)
]]>These recommendations focus on key parameters companies should consider when delivering food to consumers.
The release of food safety best practices for third-party delivery services are recommendations focused on key parameters companies should consider when delivering food to consumers. They address the safety of foods ordered online and delivered directly to consumers, which is a priority outlined in the FDA’s New Era of Smarter Food Safety blueprint.
Consumers are increasingly ordering food from a variety of online retailers, including produce and meal-kit subscription services, ghost kitchens (which only prepare and fulfill orders for delivery, without a physical storefront), and third-party delivery services and programs.
The best practices document identifies mitigating measures to potential food safety vulnerabilities, including those that may arise in the “last mile” of delivery, with the last mile referring to the final leg of the food’s journey to consumers’ homes.
This guidance document provides food safety best practices that include preventive controls, mechanisms to assess risk, recommendations for proper packaging, temperature control, physical and chemical contamination control, and allergen control.
The 49-page document provides food safety best practices for managing or performing Direct to Consumer (DTC) or third-party delivery (TPD) services.
“This document,” it says, ” includes parameters critical to preventive controls, mechanisms to assess risk, validation and verification practices, recommendations for proper packaging, temperature control, receiving and storage, physical and chemical contamination control, allergen control, general food safety information, and suggestion for return of compromised and abused products. The intent of the guide is primarily to provide best practices for preventing biological, physical, and chemical contamination as well as the growth of harmful bacteria and/or the formation of toxins within the food being transported.”
“The methods by which foods reach the final consumer can vary significantly, and this guidance is not intended to provide a “one-size-fits-all” approach,” it continues. “This guidance aims to review some of the essential parameters that any company should consider in providing safe foods to the consumer. Companies should research, understand, and test the methods best suited to their specific operation.”
CFP, a non-profit organization created in 1971, provides a formal process for the food industry, state and local health departments, academia, and consumer organizations to submit input in the development and/or modification of recommended national retail food safety policy, which is incorporated into state, local, tribal, and territorial food safety laws and regulations, upon adoption of the FDA Food Code. It also identifies and addresses emerging problems associated with food safety.
This collaboration is one example of how the FDA, in its New Era of Smarter Food Safety, is engaging with both industry and all stakeholders to help ensure food safety as new business models emerge and change to meet the needs of the modern consumer.
Another example is the three-day public meeting the FDA held in October 2021 to discuss the safety of foods ordered online and delivered directly to consumers. The response showed that this is an issue that crosses age, economic and national divides. More than 4,000 people registered to attend, and 15,400 watched online.
Additional Information:
(To sign up for a free subscription to Food Safety News, click here.)
]]>“NCC (National Chicken Council) is concerned about the precedent set by this abrupt shift in longstanding policy, made without supporting data, for a product category that has only been associated with one outbreak since 2015. It has the potential to shutter processing plants, cost jobs, and take safe food and convenient products off shelves,” according to a statement from the industry group.
The FSIS reported that since 1998, breaded and stuffed raw chicken products have been associated with up to 14 outbreaks and approximately 200 illnesses.
The National Chicken Council’s statement was issued in response to an FSIS announcement of its plans to declare Salmonella an adulterant in frozen, raw, breaded and stuffed chicken products. The chicken council statement was from Ashley Peterson, NCC’s senior vice president of scientific and regulatory affairs.
“We’re equally concerned that this announcement was not science-based or data-driven,” she said.
“Going back to the passage of the Poultry Products Inspection Act in 1957, the mere presence of Salmonella has not rendered raw poultry adulterated,” Peterson continued. “We believe FSIS already has the regulatory and public health tools to work with the industry to ensure the continued safety of these products. We’ve been asking the agency for years to collaborate on these efforts, including two petitions for stricter regulations, requests that have gone largely ignored.”
The FSIS Aug.1 policy change came with the endorsement of the head of the USDA. “Food safety is at the heart of everything FSIS does,” said Agriculture Secretary Tom Vilsack. “That mission will guide us as this important first step launches a broader initiative to reduce Salmonella illnesses associated with poultry in the U.S.”
“Today’s announcement is an important moment in U.S. food safety because we are declaring Salmonella an adulterant in a raw poultry product,” said Sandra Eskin, USDA Deputy Under Secretary for Food Safety. “This is just the beginning of our efforts to improve public health.”
By declaring Salmonella an adulterant in these products, Eskin said the FSIS will be able to ensure that highly contaminated products that could make people sick are not sold to consumers.
According to the FSIS, products in this category are found in the freezer section and include some chicken cordon bleu or chicken Kiev products. These products appear cooked, but they are only heat-treated to set the batter or breading and the products contain raw poultry. Continual efforts to improve product labeling have not been effective at reducing consumer illnesses.
As these products often appear ready to eat, but contain raw chicken, Eskin said the FSIS recognizes that their nature raises special considerations that merit additional attention.
The National Chicken Council (NCC) claims that its member companies have invested millions of dollars and have worked for more than a decade to develop and refine best practices for these products to reduce Salmonella and protect public health. The NCC says these efforts have been paying off, demonstrated by a significant decline in illness in the past seven years.
The Washington D.C.-based trade association says as these products often appear ready to eat, but contain raw chicken, it recognizes their nature raises special considerations that merit additional attention.
The FSIS says its plan for breaded and stuffed raw chicken products will be to consider the products adulterated when they exceed a very low level of Salmonella contamination and would be subject to regulatory action.
The FSIS will be proposing to set the limit at 1 colony forming unit (CFU) of Salmonella per gram for these products, a level that the agency believes will significantly reduce the risk of illness from consuming these products. The agency will seek comment on whether a different standard for adulteration — such as zero tolerance or one based on specific serotypes — would be more appropriate.
The notice, scheduled for fall publication in the Federal Register, will be seeking public comments that address what the standard should be as well as to help the agency develop a final implementation plan, including a verification testing program.
Once published, the notice will be posted on FSIS’ Federal Register & Rulemaking page for review and comment. When the proposal is finalized, the FSIS will announce its final implementation plans and the date it will begin routine testing for Salmonella in these products.
This action is part of the FSIS’ broader efforts to reduce Salmonella illnesses associated with poultry. In October 2021, the USDA announced it was reevaluating its strategy for controlling Salmonella in poultry, including whether Salmonella should be considered an adulterant in specific raw poultry products. Since launching this effort, the USDA has been focusing on gathering information by meeting with stakeholders to hear their ideas, asking for recommendations from food safety experts, and soliciting ideas for pilot projects from the industry to test drive different control strategies in poultry establishments. The USDA plans to present a proposed framework for a new comprehensive strategy to reduce Salmonella illnesses attributable to poultry in October and convene a public meeting to discuss it in November.
The NCC says the FSIS and has long interpreted the Poultry Products Inspection Act such that Salmonella is not an adulterant in raw poultry, a view reinforced by federal courts as well.
It says chicken processors take a number of steps to reduce and control Salmonella during processing, and final customary consumer cooking to an internal temperature of 165 degrees F destroys any Salmonella that may remain. The FSIS has never since the Poultry Products Inspection Act was passed in 1957, taking the view that the mere presence of Salmonella on raw poultry renders the product adulterated.
According to the NCC’s count, eleven outbreaks associated with these products have been investigated by public health officials since 1998. Prior to one 2021 outbreak, the last multistate outbreak of not-ready-to-eat stuffed chicken products was in 2015.
(To sign up for a free subscription to Food Safety News, click here.)
]]> |
The Journal of Food Proection beginning in January 2023 will be published as a fully open access publication, the International Association for Food Protection (IAFP) announced Wednesday.
IAFP said the Journal of Food Protection will be published as an open access journal with Elsevier, the Netherlands-based academic publishing company specializing in scientific, technical, and medical content. Its products include journals such as The Lancet, Cell, the ScienceDirect collection of electronic journals, Trends, the Current Opinion series, the online citation database Scopus, the SciVal tool for measuring research performance, the ClinicalKey search engine for clinicians, and the ClinicalPath evidence-based cancer care service.
A publication is defined as ‘open access’ when there are no financial, legal, or technical barriers to accessing it – that is to say when anyone can read, download, copy, distribute, print, search for and search within the information, or use it in education or in any other way within the legal agreements.
“The mission of IAFP is to provide food safety professionals worldwide with a forum to exchange information on protecting the food supply. IAFP’s decision was motivated in part by the Editorial Board’s desire to make JFP’s essential research open to all and to reach the widest audience across all its sectors in corporate, government, and education. ” according to the announcement. “As prior issues of the Journal of Food Protection older than five years were made free to read online, usage data skyrocketed, confirming a need for the content. These back files include JFP’s two prior titles: Journal of Milk and Food Technology (1947-1976) and Journal of Milk Technology (1937-1946)
“Noticeable growth in authors choosing open access indicated a desire to have their content freely available for all to read. In the current model, all authors already pay page charges. This fee will be replaced by an Article Publishing Charge of $1,600 for IAFP’s Members, for which the articles will become fully accessible upon publication. Under this model, authors can also share their research more broadly, without paywalls or copyright issues, IAFP said.
Following a full exploration and consideration of its options, the IAFP Executive Board chose to work with Elsevier based on their experience transitioning subscription journals to fully open access journals and the strength of their platform that will help increase the discovery and visibility of JFP content. The agreement will reduce the cost of open-access publishing for both Members and nonmembers.
IAFP looks forward to making all JFP research available for everyone to read, download, copy, and distribute.
(To sign up for a free subscription to Food Safety News, click here)
]]>The Centers for Disease Control and Prevention continues to estimates that every year approximately 1 in 6 people living in the U.S. — 48 million people — get sick, 128,000 are hospitalized, and 3,000 die from foodborne illness.
Local, tribal, state, territorial, and federal environmental public health and agricultural departments, agencies, and organizations make up the retail food regulatory community and are responsible for preventing and responding to foodborne illness.
“This assessment is essentially a national census of the retail food regulatory community. It is significant for both what it includes and who it surveys,” said Rance Baker, director of the Entrepreneurial Zone department at the Denver-based NEHA. “With so many competing interests pursuing the same financial resources, it is important that we determine where the training dollars are needed most. This survey will look at the intersection between curricula and needs in the retail food regulatory community to identify the gaps in the integrated food safety system.”
A comprehensive training infrastructure for retail food safety regulatory professionals is an essential component in preventing foodborne illness. The information provided in this national survey will inform decisions about food safety training and resources for years to come.
All individuals working in retail regulatory food safety are encouraged to complete the survey. It will remain open until this fall.
“Who should complete the census? Everyone in the regulatory realm of the U.S. retail food safety system,” said Baker.
For more information about the assessment, retail food safety, or the NEHA-FDA RFFM Grant Program, visit www.neha.org/retailgrants.
NEHA represents more than 6,600 governmental, private, academic, and uniformed environmental health professionals in the U.S., its territories, and internationally. NEHA is the profession’s strongest advocate for excellence in the practice of environmental health as it delivers on its mission to build, sustain, and empower an effective environmental health workforce.
(To sign up for a free subscription to Food Safety News, click here)
]]>The document provides guidance on:
- How to recognize and evaluate biological, chemical (including radiological), and physical agents that are known or reasonably foreseeable hazards in manufacturing, processing, packing, and holding of animal food,
- Ways to identify and implement preventive controls for hazards that require a preventive control in animal food,
- Components of preventive control management (e.g., monitoring, corrective actions, and verification (including validation), and
- Recordkeeping requirements associated with the food safety plan and the implementation of the food safety plan.
The FDA released draft GFI #245 in January 2018 and the agency received numerous comments from stakeholders, which were considered when finalizing the guidance.
One of the most notable changes is that, in response to stakeholder feedback, the FDA removed Appendix E: “Aid to Identifying Animal Food Hazards” and clarified that not all the hazard examples in the guidance are applicable to all animal food or all facilities. Facilities should use the hazard information in Chapter 3 of the guidance as they consider whether particular hazards are known or reasonably foreseeable for their animal food.
The FDA also added more information, resources, and examples of certain hazards in animal food, including information on animal food recalls that occurred since the draft guidance published. Lastly, the FDA made editorial and formatting changes to improve clarity and consistency.
This FSMA guidance provides detailed information to help animal food facilities anticipate possible food safety hazards, identify risk-based preventive controls to prevent or minimize those hazards, and create and implement a plan to keep unsafe animal food from entering the marketplace. Animal food facilities with questions about how this guidance applies to them can contact [email protected] for further assistance.
Additional Information
- Final Guidance for Industry #245: Hazard Analysis and Risk-Based Preventive Controls for Food for Animals
- Federal Register Notice of Availability: Hazard Analysis and Risk-Based Preventive Controls for Food for Animals; Guidance for Industry
- FSMA Final Rule for Preventive Controls for Animal Food
- Fact Sheet: Final Rule on Preventive Controls for Animal Food
- Frequently Asked Questions on FSMA
(To sign up for a free subscription to Food Safety News, click here.
]]>Yongning Wu, from the China National Center for Food Safety Risk Assessment, said countries are at different stages with their national food safety systems and a tailored approach would be needed. Foodborne disease surveillance in many nations is managed by the health sector and there can be limited links with food safety authorities and testing laboratories.
Delegates at the 75th World Health Assembly recently adopted the Global Strategy for Food Safety 2022 to 2030. The update is to ensure food safety systems are modernized and multi-sectoral collaboration is strengthened. Countries were encouraged to either develop national implementation roadmaps or use existing food safety policies and programs, and to allocate resources to the problem.
The WHO Director-General must report back on progress in implementing the plan to the World Health Assembly in 2024 and every two years until 2030.
The revised strategy aims to support countries in efforts to prioritize, plan, implement, monitor, and regularly evaluate their actions toward reducing the burden of foodborne diseases. WHO will publish guidance to help member states to implement the new strategy and develop work plans including investment cases and baseline surveys.
The Chinese government’s proposed roadmap for domestic food safety included a zero tolerance of systemic food safety risks by 2020 and improving the level of assurance and establishing a strict, efficient, and socially governed food safety system by 2027, said Wu in China CDC Weekly, as part of an issue to mark World Food Safety Day on June 7.
The strategy aims to achieve the modernization of food safety governance and oversight of the food chain by 2035 and universal modernization of food safety governance throughout China, and to be one of the leading counties for food safety standards and governance by 2050.
Choice of indicators
In the WHO strategy, indicators are used to provide information about progress toward a target so action can be taken if required. One indicator is foodborne diarrheal disease incidence per 100,000 population. The proposed target is to achieve a 40 percent reduction in the global average by 2030 compared to the 2010 baseline.
In China, there is a lack of background data for disease burden of foodborne illness and diarrheal diseases. However, an enhanced surveillance system is now in place to detect and monitor foodborne diseases and food contamination, said Wu.
China has cautioned about the interpretation of surveillance data and using it to compare countries, as this may reflect the systems and laboratory capability rather than the true incidence and prevalence of the disease.
Technical Advisory Group members suggested foodborne outbreaks might be a better indicator although there are still issues around comparability between countries because of differences in epidemiological investigative ability and surveillance systems. Foodborne diarrheal disease statistics also overlook data on chemical contamination of food.
Other ideas included using sub-indicators under the main indicators. These could focus on a country’s testing capacity, to see if it is looking for certain foodborne pathogens and identify gaps in the surveillance system.
Wu said countries might be reluctant to report data due to potential trade implications and global targets might need adapting for regional and domestic levels.
“The challenge with setting targets is that there are limited baseline studies within countries, which means that the target-setting experience in the regions is very subjective. Another important issue is that countries have different capacities, so it might be more reasonable to set different targets for different countries or regions,” he said.
(To sign up for a free subscription to Food Safety News, click here.)
]]>The man, from Grays Harbor County, was between 55 and 65 years old, according to a news release from the public health department.
The department has not yet released any other information about the man, except to say it is believed he died from botulism poisoning. Testing is ongoing to confirm the cause of death.
“Grays Harbor County Environmental Health assisted the property owner with the safe disposal of around 170 pint-sized jars of home-canned food and canning jars per CDC guidelines,” according to the county’s news release.
Botulism is odorless and cannot be seen or tasted; however, even a small taste of food containing the toxin can be deadly, according to the U.S. Centers for Disease control and Prevention, the county release warns.
The CDC’s information on home canning includes the following tips:
1. Use proper canning techniques.
The best way to prevent foodborne botulism is by carefully following instructions for safe home canning from the USDA Complete Guide to Home Canning . Only use recipes and cookbooks that follow the steps in the USDA guide. Don’t use other recipes, even if you got them from a trusted friend or family member.
You can learn more about proper home canning from these resources:
- The National Center for Home Food Preservation
- State and county extension services
(click on your state or scroll down for a list of all services)
2. Use the right equipment for the kind of food you are canning.
Low-acid foods are the most common sources of botulism linked to home canning. These foods have a pH level greater than 4.6. Low-acid foods include most vegetables including asparagus, green beans, beets, corn, tomatoes and potatoes, some fruits, milk, all meats, fish and other seafood.
Pressure canning is the only recommended method for canning low-acid foods.
- Do not use a boiling water canner for low-acid foods because it will not protect against botulism.
- Do not use an electric, multi-cooker appliance, even if it has a “canning” or “steam canning” button on the front panel. Learn more
When pressure canning, keep the following things in mind.
- Use a recommended pressure canner that holds at least four one-quart jars sitting upright on the rack.
- Be sure the gauge of the pressure canner is accurate. Many county extension offices will check gauges. Contact the pressure canner manufacturer for other options.
- Clean lid gaskets and other parts according to the manufacturer’s directions.
- Vent the pressure canner before pressurizing and follow recommended cooling steps.
- Use up-to-date processing times and pressures for the kind of food, the size of jar, and the method of packing food in the jar. Pay special attention to processing times for low-acid foods.
Review USDA’s Complete Guide to Home Canning for more information on pressure canning.
3. When in doubt, throw it out!
If you have any doubt whether safe canning guidelines have been followed, do not eat the food.
Home-canned and store-bought food might be contaminated with toxin or other harmful germs if:
- the container is leaking, bulging, or swollen;
- the container looks damaged, cracked, or abnormal;
- the container spurts liquid or foam when opened; or
- the food is discolored, moldy, or smells bad.
From Grays Harbor County Public Health:
Two resources for safe canning practices include the CDC – https://www.cdc.gov/foodsafety/communication/home-canning-and-botulism.html – and Washington State University Extension Grays Harbor – https://extension.wsu.edu/graysharbor/family/food/.
If you’re new to canning or need a refresher, the USDA has a great resource, the Complete Guide to Home Canning, available for free download at https://nchfp.uga.edu/publications/usda/GUIDE01_HomeCan_rev0715.pdf.
About botulism
While a variety of illnesses can result from eating under-processed food, one of the most dangerous is botulism poisoning. Untreated, botulism can paralyze the muscles needed for breathing, resulting in sudden death.
Anyone who has eaten any recalled products and developed signs of botulism poisoning should immediately seek medical attention, according to the U.S. Centers for Disease Control and Prevention (CDC).
“In foodborne botulism, symptoms generally begin 18 to 36 hours after eating contaminated food. However, symptoms can begin as soon as 6 hours after or up to 10 days later,” according to the CDC website.
The symptoms of botulism may include some of all of the following: double vision, blurred vision, drooping eyelids, slurred speech, difficulty swallowing, difficulty breathing, a thick-feeling tongue, dry mouth, and muscle weakness. People with botulism poisoning may not show all of these symptoms at once.
These symptoms result from muscle paralysis caused by the toxin. If untreated, the disease may progress, and symptoms may worsen to cause paralysis of specific muscles, including those used in breathing and those in the arms, legs, and the body from the neck to the pelvis area.
(To sign up for a free subscription to Food Safety News, click here)
]]>Follow these tips from the Food and Drug Administration to keep your food safe:
If the Power Goes Out
Cold temperatures slow the growth of harmful bacteria. Keeping food at safe temperatures is key to reduce the risk of foodborne illnesses.
- Keep refrigerator and freezer doors closed as much as possible. The refrigerator will keep food cold for about 4 hours, and a full freezer will keep the temperature for approximately 48 hours (24 hours if half full) if the doors remain closed.
- Use ice (dry, block ice, or ice cubes) and frozen containers of water or gel packs to keep your refrigerator and freezer as cold as possible.
- Do not rely on placing food outdoors. Temperatures can vary, especially if sunlight reaches the food even while temperatures remain low.
When Power is Restored
Before eating any food after a power outage, check the temperatures inside your refrigerator and freezer.
- If the power was out for no more than 4 hours, refrigerated food should be safe as long as the doors were kept closed. When the power comes back on, check the temperature in the refrigerator or of the food. Perishable foods such as meat, poultry, seafood, milk, eggs, or leftovers with temperatures that are 45 degrees F or below, as measured with a food thermometer, should be safe but cook and consume them as soon as possible.
- Discard any perishable food that has been at temperatures above 40 degrees F for 4 hours or more.
- If the freezer thermometer reads 40 degrees F or below, food is safe and may be refrozen. If you did not have a thermometer in the freezer, check each package to determine its safety; you can’t rely on appearance or odor. If the food still contains ice crystals or is 40 degrees F or below, it is safe to refreeze or cook.
- Be aware that perishable foods that are not kept adequately refrigerated or frozen may cause food poisoning if eaten, even after they are thoroughly cooked.
If a storm is coming, be prepared and plan ahead
- Use a refrigerator and freezer thermometer, and check it regularly to ensure that the refrigerator temperature is at or below 40 degrees F and the freezer is at or below zero degrees F.
- Plan for ice. Know where you can get dry or block ice. Make ice cubes and freeze containers of water or gel packs to help keep food cold when there is a loss of power.
- Keep coolers on hand to store refrigerated food if the power will be out for more than 4 hours.
- Freeze refrigerated items that you may not need immediately, and group foods close together in the freezer.
- Stock your pantry with a few days’ worth of ready-to-eat foods that do not require cooking or refrigeration.
And remember, there are some serious risks to storing food outside.
(To sign up for a free subscription to Food Safety News, click here.)
]]>While foodborne illnesses require specific testing to be diagnosed, a list of symptoms common to most of them gives sick people a good idea whether they might have been infected.
First, though, public health officials say it may not have been the most recently eaten meal that causes food poisoning symptoms. Many of the most common foodborne illnesses have incubation periods that can be hours, days or even several weeks.
Incubation periods for common foodborne pathogens
- Staphylococcus aureus – 1 to 8 hours, typically 2 to 4 hours
- Campylobacter – 2 to 7 days, typically 3 to 5 days
- E. coli O157:H7 – 1 to 10 days, typically 3 to 4 days
- Salmonella – 6 to 72 hours, typically 18 to 36 hours
- Shigella – 12 hours to 7 days, typically 1 to 3 days
- Hepatitis a – 15 to 50 days, typically 25 to 30 days
- Listeria – 3 to 70 days, typically 21 days
- Norovirus – 24 to 72 hours, typically 36 hours
If symptoms of a foodborne illness develop – stomach cramps, vomiting, diarrhea that is often bloody – the Centers for Disease Control and Prevention recommends the following:
- Rehydrate slowly — sips, not gulps — because drinking fluids rapidly can increase vomiting.
- Do not self-treat with anti-diarrheal medications or anti-nausea medications unless advised to do so by a medical provider — especially if you have bloody diarrhea. Some medications can slow stool transit or suppress vomiting, which can make some kinds of food poisoning worse.
- Do not take antibiotics — your own or anyone else’s — unless prescribed by a medical provider, because this can also make some kinds of food poisoning worse.
- What goes in must come out — if urine output reflects how much you are drinking, and is light colored and clear, you are probably getting enough fluids. If you stop urinating for longer then a few hours, despite drinking adequate fluids, that can be a medical emergency and you should seek medical attention immediately.
- If emergency room visits are necessary, patients should ask about specific testing to identify the pathogen that is making them ill. Food poisoning symptoms can mimic those of viruses, resulting in errors in treatment.
- If a pathogen is identified contact the local public health department and report known food exposures for the incubation period of the known pathogen.
(To sign up for a free subscription to Food Safety News, click here.)
]]>And just like sports fans need to take certain precautions to stop the spread of COVID-19, the same is true of foodborne illness.
Here are some tips for making sure your game day doesn’t end in a loss to food poisoning.
PRO Grilling
You can reduce and avoid foodborne illnesses from cooking meat or poultry on the grill by following these three PRO tips from the USDA.
 P — Place the Thermometer
P — Place the Thermometer
When you think your food is cooked, check the internal temperature by inserting a food thermometer into the thickest part of the meat, usually about 1.5 to 2 inches deep. If you are cooking a thinner piece of meat, like hamburger patties, insert the thermometer from the side. Make sure that the probe reaches the center of the meat.
- R — Read the Temperature, in due time
Keep the thermometer in place for about 10 to 20 seconds for an accurate temperature reading. Use the following safe internal temperature guidelines for your meat and poultry.
- Beef, Pork, Lamb, and Veal (steaks, roasts, chops) and Fish: 145 degrees F (63 degrees C) with a 3-minute rest time.
- Ground meats: 160 degrees F (71 degrees C)
- Whole poultry, whole and cut pieces of poultry, and ground poultry: 165 degrees F (74 degrees C)
- O — Off the Grill
Once the meat and poultry reach their safe minimum internal temperatures, take the food off the grill and place it onto a clean platter. Don’t put cooked food on the same platter that held raw meat or poultry. Also, remember to clean your food thermometer probe with hot, soapy water or disposable sanitizing wipes between uses.
Take the right equipment
Make sure to game plan and have all the proper cooking and cleaning supplies.
- Clean utensils for preparing and serving cooked food
- A food thermometer, vital for knowing that your meat and poultry reaches a high enough temperature to destroy harmful bacteria.
- An insulated cooler packed with several inches of ice, frozen gel packs, frozen water bottles, or containers of ice to carry cold perishable food like raw hamburger patties, sausages, and chicken.
- Take extra water for cleaning if none will be available at the site.
- Pack clean, wet, disposable cloths or moist towelettes and paper towels for cleaning hands and surfaces.
Keep cold food cold and hot food hot
Keeping food at a safe temperature between home, a store or restaurant, and the tailgate location helps prevent foodborne illness.
- Place an appliance thermometer on the food in the cooler so you can check to be sure the food stays at 40 degrees F or below.
- When packing the cooler for an outing, be sure raw meat and poultry are wrapped securely to prevent their juices from cross-contaminating ready-to-eat food such as raw vegetables and fruits.
- Perishable cooked food such as luncheon meat, cooked meat, chicken, and potato or pasta salads must be kept refrigerator cold, too.
- If taking hot, eat it within 2 hours — 1 hour if the temperature is above 90 degrees F.
- To keep food like soup, chili, and stew hot, use an insulated container. Fill the container with boiling water, let it stand for a few minutes, empty, and then put in the piping hot food. If you keep the insulated container closed, the food should stay hot at 140 degrees F or above for several hours.
- If you can’t keep hot food hot during the drive to your tailgate, plan ahead and chill the cooked food in the refrigerator before packing it in a cooler. Reheat the food to 165 degrees F on the grill as measured with a food thermometer. For foods such as baked beans, disposable aluminum pans work well on grills.
- Transport marinated meat and any reserved marinade in a cooler, and keep it cold until grilling.
Safely marinate
Have a backup marinade that hasn’t touched raw meat or poultry.
- Always marinate food in the refrigerator, not on the counter at room temperature.
- If some of the marinade is to be used for basting during smoking or as a sauce on the cooked food, reserve a portion of the marinade. Don’t put raw meat and poultry in it.
- Don’t reuse the marinade from raw meat or poultry on cooked food unless it’s boiled first to destroy any harmful bacteria.
- Transport marinated meat and any reserved marinade in a cooler, and keep it cold until grilling it.
Avoid cross-contamination
Cross-contamination occurs when juices from raw meat or poultry touch ready-to-eat foods, like vegetables, fruits or cooked food.
- When taking food off the grill, use a clean utensils.
- Don’t put cooked food on the same platter that held raw meat or poultry. Any harmful bacteria present in the raw meat juices could contaminate safely cooked food.
- In hot weather — above 90 degrees F, food should never sit out for more than 1 hour.
Saving the leftovers
Make sure you take the time to properly handle the food that isn’t eaten.
- Holding food at an unsafe temperature is a prime cause of foodborne illness.
- Store perishable food in the cooler except for brief times when serving.
- Cook only the amount of food that will be eaten to avoid the challenge of keeping leftovers at a safe temperature.
- Discard any leftovers that are not ice cold — 40 degrees F or below — after two hours.
(To sign up for a free subscription to Food Safety News, click here.)
]]>Whether you tried your hand at baking bread, followed a new recipe on Tik Tok, or even thought up some creative dishes “Iron Chef” style, the past 18 months have turned many more of us into home cooks. For Food Safety Education Month (FSEM) in September, we’re sharing advice on another important part of a tasty meal: How to prevent food poisoning when you cook at home.
Meet Food Safety Chef, who will share ways you can handle and keep food safe in your home kitchen. During September, follow along on social media to see these tips and share them with others: @Foodsafetygov Twitter, FoodSafety.gov Facebook, @CDCgov Twitter, @CDC_NCEZID Twitter, CDC Facebook, and CDCgov Instagram. Look for the hashtags #FSEM2021 and #CDCFoodSafety.
Safety is an ingredient for everyone
Being a chef in your own home can be fun. During Food Safety Education Month, make room for food safety in your kitchen and help educate others about preventing food poisoning. Here are some resources from the Centers for Disease Control and Prevention you can use:
- CDC’s Food Safety Education Month Page
- Social Media Messages
- Social Media Graphics
- Videos
- Charts With Food Safety Guidelines
Spotlight on Salmonella
The CDC estimates that Salmonella causes more foodborne illnesses in the United States than any other bacteria. Chicken is a major source of these illnesses, although Salmonella can contaminate a variety of foods. Large Salmonella outbreaks linked to ground beef have also occurred in recent years. Federal agencies and their partners are working along the food chain to prevent Salmonella illnesses associated with chicken and ground beef.
You can help prevent Salmonella and other foodborne infections by following food safety advice while preparing your favorite chicken and ground beef dishes. Try a recipe for spice-crusted chicken that includes food safety steps.
Add these steps to all your recipes to make your meals delicious and safe.
Get cooking: Food Safety Chef’s 4-step recipe for food safety
- Clean: Wash your hands often. Clean your counters with hot soapy water, but don’t wash your chicken or meat! Washing raw meat, chicken, turkey, fish or eggs can spread germs to your sink, countertops, and other surfaces in your kitchen.
- Separate: Keep raw meat, chicken, turkey, seafood, and eggs separate from other foods. Use different cutting boards for uncooked meats and vegetables to avoid germs from raw meat contaminating food that won’t be cooked before you eat it.
- Cook: Cook foods to a safe internal temperature to kill germs that could make you sick. Measure with a food thermometer because you can’t tell if food is fully cooked just by looking at the color.
- Chill: Refrigerate your leftovers and other perishable food within 2 hours of cooking. If it’s warmer than 90 degrees F outside, refrigerate leftovers after only an hour. Keep your refrigerator at 40 degrees F or below.
(To sign up for a free subscription to Food Safety News, click here.)
]]>Labor Day often signals the end of summer for many in the United States, and the end of summer vacation for children of all ages. It is always the perfect time for friends and family to pause and spend some time together before heading back to work or a busy school schedule.
But if people aren’t careful and follow food safety basics, getting back to school or work could be put in jeopardy by food poisoning.
Cooling and packing food
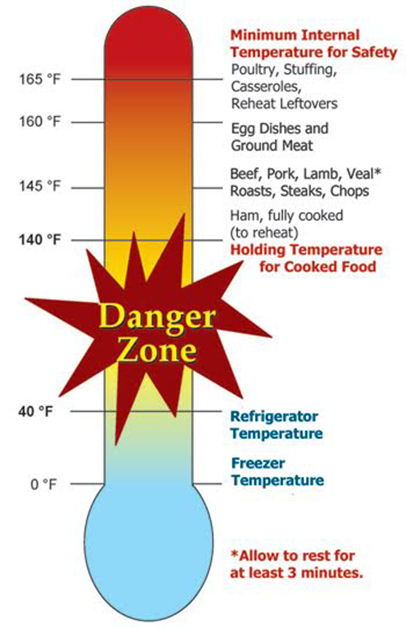
Most foods that are prepared for outdoor gatherings are not properly cooled, according to public health officials. Not cooling just-cooked food quick enough allows harmful bacteria to multiply rapidly. Once cooked food has been properly cooled, it should be placed in a shallow container for immediate refrigeration until it is packed for transportation
Washing fruits and vegetables
Commonly forgotten, cutting through the peels and rinds of fruit, such as apples or melons, can transfer bacteria into the flesh of the fruit. All fruits and vegetables to be served raw should be washed before they are cut. The cut produce should be refrigerated in waterproof containers or plastic wrap to cool down before going into the picnic cooler.
Cooler location
Once foods reach their destination, they are often left to sit out in warm temperatures for too long. It’s a good idea to put coolers in the passenger area of a car rather than the trunk where temperatures are usually higher. Once the cooler reaches the picnic site, place it in the shade with a blanket over the top and keep the cooler closed until it’s time to eat.
Cold foods cold, hot foods hot
Cold foods should be kept cold and hot foods should be kept hot to reduce the chance of bacteria and other pathogens multiplying. Ice and frozen gel packs are a necessary addition to coolers and insulated storage containers. To keep foods hot, the USDA recommends filling heat-safe, insulated containers with boiling water. After letting the boiling water stand for a few minutes, empty it out and replace with hot soup, chili or stews. These containers should remain closed or covered until it’s time to eat.
Handling food and handwashing
The more hands that handle the hamburgers, hotdogs, salads and other foods, the more possibility for contamination. People that handle food from preparation to plate should always thoroughly wash their hands to avoid the spread of bacteria. If running water is not available at your outdoor meal, hand sanitizers and paper towels should be used liberally, but they are not as effective. Use the sanitizer and wipe hands with clean paper towels. Then use the sanitizer a second time and let your hands air dry.
Utensils and dishes should be plentiful to avoid cross-contamination from preparing meat, poultry or fish on the same dish before and after cooking. Disposable plates and utensils are a great option if dishes cannot be washed in between preparation and completion of cooking.
PRO Grilling
You can reduce and avoid foodborne illnesses from cooking meat or poultry on the grill by following these three tips from the USDA.
- P — Place the Thermometer
When you think your food is cooked, check the internal temperature by inserting the thermometer into the thickest part of the meat, usually about 1.5 to 2 inches deep. If you are cooking a thinner piece of meat, like hamburger patties, insert the thermometer from the side. Make sure that the probe reaches the center of the meat.
- R — Read the Temperature, in due time
Wait about 10 to 20 seconds for an accurate temperature reading. Use the following safe internal temperature guidelines for your meat and poultry.
-
- Beef, Pork, Lamb, and Veal (steaks, roasts, chops) and Fish: 145 degrees F (63 degrees C) with a 3-minute rest time.
- Ground meats: 160 degrees F (71 degrees C)
- Whole poultry, whole and cut pieces of poultry, and ground poultry: 165 degrees F (74 degrees C)
- O — Off the Grill
Once the meat and poultry reach their safe minimum internal temperatures, take the food off the grill and place it onto a clean platter. Don’t put cooked food on the same platter that held raw meat or poultry. Also, remember to clean your food thermometer probe with hot, soapy water or disposable sanitizing wipes between uses.
(To sign up for a free subscription to Food Safety News, click here.)
]]>However, this can lead to certain risks that should be avoided.
Here are some answers to common food safety questions from students and their parents from the United States Department of Agriculture Food Safety and Inspection Service:
Q: Several slices of pizza have been left out overnight. Is the pizza still safe to eat?
A: No. Perishable food should never be left out of refrigeration for more than two hours. This is true even if there are no meat products on the pizza. Foodborne bacteria that may be present on these foods grow fastest at temperatures between 40 degrees F and 140 degrees F and can double in number every 20 minutes.
Other takeout or delivered foods such as chicken, hamburgers, cut fruit, salads and party platters, must also be kept at a safe temperature. The rule is to “keep hot food hot and cold food cold” To keep hot foods safe, keep them at 140 degrees F or above. Cold food must be kept at 40 degrees F or below in the refrigerator or freezer. Bacteria grow rapidly between 40 degrees F and 140 degrees F. Discard all perishable food left at room temperature longer than 2 hours; 1 hour in air temperatures above 90 degrees F. Use safely refrigerated food in 3 to 4 days; frozen leftovers, 1 to 2 months.
Q: I am living off-campus this year. My two roommates and I will be preparing our own meals. What do we need to know to cook food safely?
A: When using frozen meats, thaw them in the refrigerator — not on the counter. Don’t allow raw meat or poultry juices to drip on other foods. Wash your hands before and after preparing foods. Always use clean paper towels. Wash used cutting boards and utensils in hot, soapy water. Use a food thermometer to check internal temperatures. Cook hamburger and other ground meats (veal, lamb, and pork) to an internal temperature of 160 degrees F and ground poultry to 165 degrees F. Beef, veal and lamb steaks and roasts may be cooked to 145 degrees F for medium-rare. Whole poultry should be cooked to 180 degreed F as measured in the thigh; breast meat to 170 degrees F. All cuts of pork should reach 160 degrees F. Foods from the microwave should be steaming hot and checked with a food thermometer. Finally, if you feel food has not been handled safely, throw it out.
Q: I don’t have a car on campus so I have to take the bus to get my groceries. Will the food be safe by the time I get it to my apartment?
A: Whether you use public transportation or have your own car, it’s important that perishable purchases are refrigerated within 2 hours (1 hour when the temperature is above 90 degrees F). First, when buying food, avoid cross-contamination by placing raw meat, poultry, and seafood in plastic bags and keep them separate from other foods in your grocery shopping cart. Make cold foods the last items you place in your cart. After your purchases are bagged, go home immediately. If you can’t get home within the recommended times, you may want to take a cooler with frozen gel packs to keep perishable food safe in transit. If there are perishable raw meats you don’t plan on using soon, freeze any ground meats, poultry or fish within 2 days; beef, pork, veal or lamb steaks, roasts or chops within 3 to 5 days.
Q: Our dorm has a kitchen with a microwave on each floor. When I microwave the food according to the package’s instructions, it’s still partly frozen. Why doesn’t it get hot enough?
A: In a large building like a dorm, electrical equipment such as computers, toaster ovens, hairdryers and irons compete for current and reduce the electrical wattage of a microwave. A community oven that has been used just before you, will cook slower than a cold oven. To compensate, set the microwave for the maximum time given in the instructions. Avoid using an extension cord with the microwave because power is reduced as it flows down the cord. Also, the cord might not be grounded. Cover foods during cooking. Remember to stir or rearrange food and rotate the dish. Allow for standing time: the food continues to cook during this period. Finally, use a food thermometer to ensure the food reaches the safe internal temperature of 165 degrees F. If the food has not reached that temperature or is not steaming hot, add more cooking time.
Q: What containers are safe for microwaving foods?
A: Plastic cold-storage containers such as margarine tubs, takeout containers, whipped topping bowls and other one-time use containers should not be used in microwave ovens. These containers can warp or melt, possibly causing harmful chemicals to migrate into the food. Microwave plastic wraps, wax paper, cooking bags, parchment paper, and white microwave-safe paper towels should be safe to use. Do not let plastic wrap touch foods during microwaving. Never use thin plastic storage bags, brown paper or plastic grocery bags, newspapers, or aluminum foil in the microwave oven.
Q: How do you thaw frozen foods in the microwave safely?
A: Remove food from packaging before defrosting. Do not use foam trays and plastic wraps because they are not heat stable at high temperatures. Melting or warping may cause harmful chemicals to migrate into food. Cook meat, poultry, egg casseroles, and fish immediately after defrosting because some areas of the frozen food may begin to cook during the defrosting time. Do not hold partially cooked food to cook later.
Q: Several of us are planning a tailgate party at the stadium. How can we handle the foods safely?
A: Keeping food safe from home, a store or restaurant to the stadium helps prevent foodborne illness. If bringing hot takeout food, eat it within 2 hours of purchase. To keep food like soup, chili and stew hot, use an insulated container. Fill the container with boiling water, let it stand for a few minutes, empty, and then put in the piping hot food. Keep the insulated container closed and the food should stay at a safe 140degrees F or above for several hours.
Or, plan ahead and chill the food in your refrigerator before packing for your tailgate. Carry cold perishable food like raw hamburger patties, sausages, and chicken in an insulated cooler packed with several inches of ice, frozen gel packs, or containers of frozen water. Perishable cooked food such as luncheon meat, cooked meat, chicken, and potato or pasta salads must be kept refrigerator cold, too. Tuck an appliance thermometer into the cooler to make sure the food stays at 40 degrees F or below.
When packing the cooler for an outing, be sure raw meat and poultry are wrapped securely to prevent their juices from cross-contaminating ready to-eat food. In addition to a grill and fuel for cooking food, pack a food thermometer to be sure the meat, poultry, and casseroles reach a high enough temperature to destroy harmful bacteria that may be present (see temperatures above). Include lots of clean utensils, not only for eating but also for serving the safely cooked food. Bring water for cleaning if none will be available at the site. Pack clean, wet, disposable cloths or moist towelettes and paper towels for cleaning hands and surfaces.
Q: How long will food stay safe at a tailgate party?
A: It’s important to keep hot food hot and cold food cold. Bacteria multiply rapidly between 40 degrees F and 140 degrees F. Never leave food in this “Danger Zone” more than 2 hours, 1 hour when the outside temperature is above 90 degrees F. Cook meat and poultry completely. Partial cooking of food ahead of time allows bacteria to multiply to the point that subsequent cooking cannot destroy them.
Meat and poultry cooked on a grill often browns very fast on the outside, so use a food thermometer to be sure they are cooked throughly all the way through. Cook hamburgers, sausage and other ground meats (veal, lamb and pork) to an internal temperature of 160 degrees F and ground poultry to 165 degrees F. Beef, veal and lamb steaks and roasts may be cooked to 145 degrees F for medium-rare. Poultry breast meat should be cooked to 170 degrees F and dark meat to 180 degrees F. All cuts of fresh pork should reach 160 degrees F; fully cooked ham, 140 degrees F.
Q: Are leftovers from a tailgate party safe to eat later?
A: Some people have so much fun at tailgate gatherings, they never actually make it into the stadium to see the football game. But that doesn’t mean it’s safe for the food to stay unrefrigerated before, during and after the game. Store perishable food in the cooler except for brief times when serving. Cook only the amount of food that will be eaten to avoid the challenge of keeping leftovers at a safe, high temperature. Discard any leftovers that are not ice cold after the game. Food should not be left out of the cooler or off the grill more than 2 hours or 1 hour when the outside temperature is above 90 degrees F. Holding food at unsafe temperatures is a prime cause of foodborne illness.
Q: I don’t have time to go to the dining hall for lunch. How can I safely pack a lunch to eat between classes?
A: Insulated, soft-sided lunch boxes or bags are best for keeping perishable food cold, but metal or plastic lunch boxes and paper bags can also be used. If using paper lunch bags, create layers by double bagging to help insulate the food. An ice source, such as a small frozen gel pack or frozen juice box, or frozen bottle of water should be packed with perishable food in any type of lunch bag or box. Of course, if there’s a refrigerator available, store perishable items there upon arrival. It’s important to keep perishable food cold. Harmful bacteria multiply rapidly in the “Danger Zone” — the temperatures between 40 degrees F and 140 degrees F. So, perishable food transported without an ice source won’t stay safe long. Prepackaged combos that contain luncheon meats along with crackers, cheese, and condiments must also be kept cold. This includes luncheon meats and smoked ham that are cured or contain preservatives.
Q: My math club is having a potluck dinner. What’s important to remember for food safety?
A: When you serve food, use clean containers and utensils to store and serve food. Do not use a plate or utensils previously used with raw meat, poultry, or seafood unless they have first been washed in hot, soapy water. When a dish is empty or nearly empty, replace it with a fresh container of food, removing the previous container. Place cold food in containers on ice. Hold cold foods at or below 40 degrees F. Food that will be portioned and served on the serving line should be placed in a shallow container. Place this container inside a deep pan filled partially with ice to keep food cold.
Food like chicken salad and desserts in individual serving dishes can also be placed directly on ice, or in a shallow container set in a deep pan filled with ice. Drain off water as ice melts and replace ice frequently. Keep hot food hot by using a heat source. Once food is thoroughly heated on stovetop, oven or in microwave oven, place it in chafing dishes, preheated steam tables, warming trays and/or slow cookers. Check the temperature frequently to be sure food stays at or above 140 degrees F.
Q: My buddies and I are going on a camping trip over the weekend. How can we take food along safely?
A: If you are traveling with cold foods, take a cooler with a cold source. If you are cooking, use a hot campfire or portable stove. It is difficult to keep food hot without a heat source when traveling, so it’s best to cook foods before leaving home, refrigerate or freeze the food overnight, and transport it cold. If you don’t want to lug a cooler or portable stove, consider taking shelf-stable food. Advances in food technology have produced relatively lightweight staples that don’t need refrigeration or careful packaging. These include dehydrated foods; beef jerky and other dried meats; dried noodles and soups; peanut butter in plastic jars; canned ham, chicken, beef and tuna; juice boxes; dried fruits and nuts; and powdered milk and fruit drinks. Don’t drink water from a lake or stream, no matter how clean it appears. Take bottled or tap water for drinking.
Food safety tips for parents:
Q: I frequently send “care packages” to my son at college. What other foods besides cookies, crackers and candy can I mail?
A: College students away from home always love receiving their favorite home-baked goods: Brownies and loaf-type cakes, like banana bread, carrot, applesauce or sour cream cakes, ship well if wrapped in aluminum foil and packed in a can or heavy cardboard box. Shelf-stable, microwavable entrees are another option. These foods are not refrigerated or frozen and will stay fresh without refrigeration for about 18 months. Canned meats and fish as well as dried meat and poultry, such as beef and turkey jerky, are safe to mail. Bacteria can’t grow in foods preserved by removing moisture. If mailing perishable foods, pack them with a cold source, such as frozen gel packs or dry ice, and ship them by overnight delivery. Perishables must not be at temperatures between 40 degrees F and 140 degrees F for longer than 2 hours (1 hour when the temperature is above 90 °F). Pathogenic bacteria can grow rapidly at these temperatures but they do not generally affect the taste, smell or appearance of a food. So if food has been mishandled or is unsafe to eat, the student will not be able to tell it’s dangerous.
Q: My daughter’s college is only a four-hour drive away, so she comes home often. How can I safely pack home-cooked foods for her to take back to school?
A: For a four-hour drive, food must be handled properly to keep it safe from spoilage and pathogenic bacteria. Cooked foods should be divided into shallow containers and cooled in the refrigerator before the trip. To transport the food, place it in an insulated cooler packed with several inches of ice, frozen gel packs or containers of frozen water. Add the cold containers of food from the refrigerator when she’s ready to leave. Freezing foods before the return trip also helps keep food safe. Advise your daughter to refrigerate the food as soon as she arrives at college.
(To sign up for a free subscription to Food Safety News, click here.)
]]>The Cold Chain Federation said the guidance should make it easier for members to develop, improve and implement food safety plans and processes. The guide was produced with support from the federation’s members and the UK’s Food Standards Agency.
It brings together information on compliance, best practices and recommendations for managing food safety risks in the cold chain and insights into likely future issues.
Help companies and regulatory bodies
Ensuring Food Safety in the Cold Chain has nine chapters and indicates what measures are mandatory under food safety legislation, good practices for the BRCGS Global Standard for Storage and Distribution (Issue 4), and can be used by members to check processes, as part of staff training and to obtain the highest BRCGS Storage and Distribution certification grade.
Tom Southall, Cold Chain Federation policy director, said the guide aims to help businesses achieve high standards of food safety in their facilities and to support enforcement agencies to better understand specific functions of the cold chain.
“Keeping frozen and chilled food safe is the fundamental purpose of the cold chain. Whilst the UK’s cold chain businesses are experts in keeping the nation supplied with safe food, rapidly evolving innovations and changing consumer demands makes can make maintaining these standards challenging. This can require a lot of time spent getting to grips and staying up to date with a range of regulations, certification schemes, and best practice,” he said.
Topics covered include food safety culture, Hazard Analysis and Critical Control Points (HACCP) in the cold chain, temperature control, preventing and responding to contamination, food allergens, good hygiene practices and defense against food crime.
BRCGS backing
Shane Brennan, Cold Chain Federation chief executive, said with the exit of the UK from the European Union and new trade arrangements, changes can be expected in global food supply chains.
“At the same time, the COVID-19 pandemic has extended the cold chain to the consumer’s front door. Food safety compliance systems need to be resilient, agile and forward-facing to ensure that good standards maintain safe food throughout the entire food chain from beginning to end, whatever new challenges we are faced with,” he said.
The document will be made available as part of BRCGS’s online library platform for sites and certification bodies subscribed to the BRCGS Global Standard for Storage and Distribution.
Jon Murthy, BRCGS head of global marketing, said the emphasis is on improving performance rather than compliance with minimum standards.
“The global pandemic has placed supply chain resilience firmly front of mind for brands and retailers. It has accelerated the changing role of the warehousing and logistics sector with the growth of e-commerce, the diversification of operational activities and new transport flows,” he said.
A copy can be requested by emailing: [email protected]
(To sign up for a free subscription to Food Safety News, click here)
]]>The guide aims to help nations identify food safety system needs and data gaps so they can strengthen national infrastructure and better protect public health.
It does not cover chemical hazards, including food allergens. Data requirements and methods for these hazards will be dealt with in a future publication.
Dr. Tedros Adhanom Ghebreyesus, WHO Director-General, said the handbook will help countries collect and analyze data to inform investments in food safety.
“WHO will continue to work with partners with a one health approach to keep communities safe from foodborne disease,” he said.
New stats by 2025
Figures published in 2015 estimated there were 600 million cases of foodborne illness and 420,000 deaths in 2010. Children younger than 5 years old are particularly at high risk as 120,000 of them die from unsafe food.
There are more than 250 different food hazards that cause various health issues such as acute or long-term illness or even death. This first report looked at the global public health burden of infections based on 31 foodborne hazards.
WHO is updating the burden of foodborne diseases with estimates of incidence, mortality and disease burden expected by 2025. The organization is also accepting comments on its food safety strategy until June 18.
The Foodborne Disease Burden Epidemiology Reference Group (FERG) has been renewed with 26 experts until 2024 including Beau B. Bruce of the CDC, Sandra Hoffmann from the U.S. Department of Agriculture, Elaine Scallan Walter at the Colorado School of Public Health and Felicia Wu of Michigan State University.
Foodborne diseases are preventable but this depends on informed policy-making, political commitment, and effective intervention strategies focused on the main problems, according to WHO officials.
Webinar on guide in late June
Results from country specific burden of disease estimate studies will provide the evidence needed to rank and prioritize risks, allocate resources and prevention measures, support the development of national risk-based food safety systems, and promote participation in setting international food standards.
Such work has already been done in Albania, Japan, Thailand and Uganda. Issues found included data gaps, the need for different authorities to provide access to data, and strengthening capacity of microbiological and chemical laboratories.
Foodborne Disease Epidemiology, Surveillance and Control in African LMIC (FOCAL) is a project funded by the Bill and Melinda Gates Foundation and the UK’s Department for International Development until October 2022. It will estimate the burden of foodborne diseases in Ethiopia, Mozambique, Nigeria and Tanzania.
A 90-minute webinar to discuss the guide on June 29 will be moderated by Francesco Branca, director in the department of nutrition and food safety. Other speakers are Rob Lake, from the Institute of Environmental Science and Research Limited in New Zealand; Sara Pires, of the National Food Institute in Denmark; Amare Ayalew, at the African Union Commission and Lapo Mughini Gras, from the National Institute for Public Health and the Environment (RIVM) in the Netherlands.
(To sign up for a free subscription to Food Safety News, click here.)
]]>Organic is a way to grow food following specific rules and guidelines, according to a document published by the FAO Regional Office for Asia and the Pacific. Organic certification refers to a product made in line with certain standards throughout the production, handling, processing and marketing stages; it does not cover the characteristics of the finished item.
Such standards and regulations may differ between and among countries’ supply chains for regulating chemical use and other requirements for soil and water quality maintenance.
The agency says the aim of organic food is better incomes for small-scale farmers and increased food security, environmental benefits such as enhanced soil and water quality and biodiversity preservation, and improved animal welfare.
Pesticide use
The U.S. organic sector saw food sales hit $50.1 billion in 2019, up 4.6 percent from the previous year, according to the Organic Trade Association.
Organic agriculture is seen as a promising approach to address challenges raised by increasing demographics and urbanization as well as climate change. For consumers, this often translates into healthier, safer, tastier and more environmentally friendly foods, organic proponents contend.
Organic labels rely on rules that prohibit or limit use of some synthetic fertilizers and agrochemicals, which is attractive for consumers. Pesticides produced by plants are still used in organic agriculture, which at high dosages may have negative effects on human health. The major difference is the type of pesticides used. The document stated that conventional and organic farmers need to follow the same safety standards.
From 172 countries in a survey by the Research Institute of Organic Agriculture, 87 had organic standards, and another 18 were developing legislation for them.
The FAO reported authorities could check that food safety measures are included in any existing organic certification schemes at the national level and organize a forum with the organic food industry to discuss approaches to ensuring inclusion of food safety actions in organic agriculture.
Food allergen advice
Meanwhile, the FAO has also published a document with examples of practices to establish labeling regulations for food allergens.
National contexts can differ in terms of predominance of food allergies. The FAO report says investigation is needed within countries to understand what foods should be labelled, and determine the allowable quantities of allergens that may unintentionally be present in foods.
Food allergens recognized by Codex may not cover all those that have an impact on different populations, such as the case for buckwheat in Japan.
Three case studies are presented: Japan, Australia and New Zealand, and the U.S’s Food Allergen Labeling and Consumer Protection Act (FALCPA).
The guide also covers unintentional introduction of a food allergen in a product through cross-contamination, recalls due to undeclared allergens and precautionary labeling.
National agencies were advised to regularly monitor common food allergies, ensure clarity and readability of labels and provide education on how to read them and work with the private sector, particularly e-commerce platforms and restaurants, to ensure allergens are explained to customers.
(To sign up for a free subscription to Food Safety News, click here.)
]]>Eggs can cause food poisoning because salmonella is a common bacteria found in uncooked and unbroken eggs. Salmonella can be present on both the outside and the inside of eggs.
The FDA has put regulations in place to help prevent contamination of eggs on the farm and during shipping and storage, but consumers also play a key role in preventing illness linked to eggs.
With Easter comes more egg handling, especially for children. This means it is important to follow safe handling tips when preparing, storing and serving eggs — or foods that contain them.
Here are some important food safety tips to remember after the Easter eggs festivities:
Inspect the eggs
- Cracked eggs should not be consumed, as dangerous bacteria may have entered through the crack.
Wash your hands, counters, and utensils
- This past year has taught us about the importance of washing your hands to prevent illness, and handwashing is just as important when it comes to handling eggs.
- Everybody, including children, should wash their hands with soap and water before and after handling eggs. This includes prepping, cooking, cooling, dyeing, hiding, hunting and peeling them.
- Thoroughly wash utensils, countertops and anything else the eggs come into contact with.
The safest way to boil eggs
- Place eggs in a pan of room-temperature water with the eggs covered with at least one inch of water.
- When the water is at a full boil, remove the pan from the heat source and let the eggs stay in the water for between 12-18 minutes, depending on the size of the eggs.
- After the eggs have set for the appropriate amount of time, run cold water over them.
- When the eggs are cool enough to handle, place them in the refrigerator.
Refrigerate eggs at 40 degrees F or below
- Store eggs inside the fridge, not the fridge door.
- Hard-cooked, refrigerated eggs can be stored for up to one week and safely consumed.
- Eggs — and foods containing boiled eggs — can be out of refrigeration for two hours (when it’s under 90 degrees F) and still be safe to eat.
- Even though eggs can show signs of spoilage when they’re past the best-by date, this should not be used as an indicator of an egg’s safeness — eggs that harbor Salmonella taste, smell, and appear exactly the same as “normal” eggs.
Easter eggs
- If you plan on consuming decorated eggs, make sure only food-safe dyes were used.
- The total time for hiding and hunting eggs should not exceed two hours. If the hidden eggs were out longer than two hours they should be discarded.
- Make sure hidden eggs did not come in contact with pets, wild animals, birds or lawn chemicals. Eating eggs that have been on the ground is not recommended.
- If you are planning to use colored eggs as decorations for centerpieces, etc., and the eggs will be out of refrigeration for many hours or several days, discard them after they have served their decorative purpose.
About Salmonella infections
Food contaminated with Salmonella bacteria does not usually look, smell or taste spoiled. Anyone can become sick with a Salmonella infection. Infants, children, seniors, and people with weakened immune systems are at higher risk of serious illness because their immune systems are fragile, according to the Centers for Disease Control and Prevention.
Anyone who has handled live poultry and developed symptoms of Salmonella infection should seek medical attention. Sick people should tell their doctors about the possible exposure to Salmonella bacteria because special tests are necessary to diagnose salmonellosis. Salmonella infection symptoms can mimic other illnesses, frequently leading to misdiagnosis.
Symptoms of Salmonella infection can include diarrhea, abdominal cramps, and fever within 12 to 72 hours after eating contaminated food. Otherwise, healthy adults are usually sick for four to seven days. In some cases, however, diarrhea may be so severe that patients require hospitalization.
Older adults, children, pregnant women, and people with weakened immune systems, such as cancer patients, are more likely to develop a severe illness and serious, sometimes life-threatening conditions.
Some people get infected without getting sick or showing any symptoms. However, they may still spread the infections to others.
(To sign up for a free subscription to Food Safety News, click here.)
]]>This week, many will enjoy a delicious meal on Thanksgiving Day with family and friends — either in person or virtually. Taking the necessary steps toward safe food handling and sanitation will help protect you and your loved ones this year. To make sure your Thanksgiving meal is prepared safely, the U.S. Department of Agriculture (USDA) is offering food safety advice to reduce foodborne illness, including on Thanksgiving Day.
“Our data shows that consumers can reduce their likelihood of foodborne illness by focusing on good hand hygiene and other food safety practices,” said Mindy Brashears, USDA’s Under Secretary for Food Safety. “As home chefs nationwide prepare their Thanksgiving meals, proper handwashing and avoiding cross contamination in the kitchen are critical to keeping your loved ones safe.”
Wash your hands
The first step to safe food preparation is to clean. In recent USDA observational research, participants did not even attempt to wash their hands, or did not wash their hands sufficiently about 95 percent of the time before and during meal preparation.
Handwashing is recommended to control the spread of germs, especially before, during and after preparing food, especially after touching raw meat or poultry.
 Thawing the turkey
Thawing the turkey
Frozen turkeys should never be thawed on the counter or in hot water and must not be left at room temperature for more than two hours. The best method to thaw the turkey is in the refrigerator since this allows slow, safe thawing. When thawing turkey in the refrigerator, allow about 24 hours for every five pounds of turkey. Once thawed, it can remain safe in the fridge for one to two days.
Other safe thawing methods include a cold-water bath or the microwave. If you use either of these thawing methods, you should cook the turkey immediately after it is thawed. If using the cold-water method, allow 30 minutes per pound, and submerge the turkey in its original wrapping to avoid cross-contamination. If thawing in the microwave, make sure to follow the manufacturer’s instructions when defrosting the turkey.
Avoid cross-contamination
In a recent study, USDA found 60 percent of kitchen sinks were contaminated with germs after study participants washed or rinsed poultry. To avoid this cross-contamination risk, do not wash your turkey. But if you do wash your turkey or put your turkey in the sink, you need to fully clean and sanitize your sink.
Cleaning and sanitizing is a two-step process. To clean, rub down surfaces — including the sink, cutting boards, and counter tops — with soap and hot water, and then sanitize them with a cleaning solution to remove any residual germs you cannot see. You can use a homemade solution of one tablespoon of unscented, liquid chlorine bleach in one gallon of water. Let air dry.
Do not stuff the turkey
Although many choose to stuff the turkey, USDA does not recommend doing so for optimal safety. Instead, cook stuffing outside of the turkey cavity to reduce cross-contamination risk. This will also allow your turkey to cook more quickly.
Cooking to the safe temperature
A whole turkey is safe when cooked to a minimum internal temperature of 165 degrees Fahrenheit as measured by a food thermometer in three parts: the thickest part of the breast, the innermost part of the wing, and the innermost part of the thigh.
Even if the turkey has a pop-up temperature indicator, you should still use a food thermometer to check that the bird has reached at least 165 degrees Fahrenheit in those three places. If you are planning to cook a turkey breast instead of a whole turkey, check the temperature with the food thermometer to make sure it is at least 165 degrees F at the thickest part the breast. All previously cooked side dishes should be reheated to 165 degrees Fahrenheit as measured by a food thermometer as well.
The 2-hour rule
To make sure food stays safe to eat through the weekend, all perishable items should be refrigerated within two hours of when they finished cooking. After two hours, perishable food will be in the Danger Zone (40 to 140 degrees Fahrenheit) too long, which is when bacteria can multiply quickly and cause the food to become unsafe. If foods have been left out for more than two hours they should be discarded.
Store and reheat leftovers
Store leftovers in small, shallow containers in the refrigerator until the Monday after Thanksgiving Day or in the freezer for later use. Shallow containers help cool leftovers more quickly than storing them in large containers. Reheat leftovers to an internal temperature of 165 degrees F. Check the internal temperature of the food in several places with a food thermometer after allowing a resting time.
You have questions, USDA has answers
For advice about how to safely prepare the turkey and all other menu items this Thanksgiving Day, call the USDA Meat and Poultry Hotline at 888-MPHotline (888-674-6854) or chat live with a food safety expert at ask.usda.gov from 10 a.m. to 6 p.m. EST, Monday through Friday. If you need last-minute help on Thanksgiving Day, the USDA Meat and Poultry Hotline is open from 8 a.m. to 2 p.m. EST. Visit FoodSafety.gov or follow USDA’s Food Safety and Inspection Service (FSIS) on Twitter @USDAFoodSafety or on Facebook at Facebook.com/FoodSafety.gov for the latest food safety tips.
(To sign up for a free subscription to Food Safety News, click here.)
]]>Contributed
Editor’s note: Even if you have already made holiday plans, it’s not to late to change them to reduce the chance of contracting or spreading the coronavirus.
The COVID-19 pandemic has been stressful and isolating for many people. Gatherings during the upcoming holidays can be an opportunity to reconnect with family and friends. This holiday season, consider how your holiday plans can be modified to reduce the spread of COVID-19 to keep your friends, families, and communities healthy and safe.
Unfortunately, the COVID-19 epidemic is worsening, and small household gatherings are an important contributor to the rise in COVID-19 cases. CDC offers the following considerations to slow the spread of COVID-19 during small gatherings. These considerations are meant to supplement—not replace—any state, local, territorial, or tribal health and safety laws, rules, and regulations with which all gatherings must comply.
Considerations for small gatherings of family and friends

Celebrating virtually or with members of your own household (who are consistently taking measures to reduce the spread of COVID-19) poses the lowest risk for spread. In-person gatherings that bring together family members or friends from different households, including college students returning home, pose varying levels of risk.
Organizers and attendees of larger events should consider the risk of virus spread based on event size (number of attendees and other factors) and take steps to reduce the possibility of infection, as outlined in the Considerations for Events and Gatherings.
There are several factors that contribute to the risk of getting and spreading COVID-19 at small in-person gatherings. In combination, these factors will create various amounts of risk:
- Community levels of COVID-19 – High or increasing levels of COVID-19 cases in the gathering location, as well as in the areas where attendees are coming from, increase the risk of infection and spread among attendees. Family and friends should consider the number of COVID-19 cases in their community and in the community where they plan to celebrate when deciding whether to host or attend a gathering. Information on the number of cases in an area can often be found on the local health department website.
- Exposure during travel – Airports, bus stations, train stations, public transport, gas stations, and rest stops are all places travelers can be exposed to the virus in the air and on surfaces.
- Location of the gathering – Indoor gatherings, especially those with poor ventilation (for example, small enclosed spaces with no outside air), pose more risk than outdoor gatherings.
- Duration of the gathering – Gatherings that last longer pose more risk than shorter gatherings. Being within 6 feet of someone who has COVID-19 for a cumulative total of 15 minutes or more greatly increases the risk of becoming sick and requires a 14-day quarantine.
- Number and crowding of people at the gathering – Gatherings with more people pose more risk than gatherings with fewer people. CDC does not have a limit or recommend a specific number of attendees for gatherings. The size of a holiday gathering should be determined based on the ability of attendees from different households to stay 6 feet (2 arm lengths) apart, wear masks, wash hands, and follow state, local, territorial, or tribal health and safety laws, rules, and regulations.
- Behaviors of attendees prior to the gathering – Individuals who did not consistently adhere to social distancing (staying at least 6 feet apart), mask wearing, handwashing, and other prevention behaviors pose more risk than those who consistently practiced these safety measures.
- Behaviors of attendees during the gathering – Gatherings with more safety measures in place, such as mask wearing, social distancing, and handwashing, pose less risk than gatherings where fewer or no preventive measures are being implemented. Use of alcohol or drugs may alter judgment and make it more difficult to practice COVID-19 safety measures.
Certain people should not attend holiday gatherings in person
People with or exposed to COVID-19 should not host or participate in any in-person gatherings if you or anyone in your household:
- Has been diagnosed with COVID-19 and has not met the criteria for when it is safe to be around others
- Has symptoms of COVID-19
- Is waiting for COVID-19 viral test results
- May have been exposed to someone with COVID-19 in the last 14 days
- Is at increased risk of severe illness from COVID-19
Do not host or attend gatherings with anyone who has COVID-19 or has been exposed to someone with COVID-19 in the past 14 days.
People at increased risk for severe illness
If you are an older adult or person with certain medical conditions who is at increased risk of severe illnessfrom COVID-19, or live or work with someone at increased risk of severe illness, you should avoid in-person gatherings with people who do not live in your household.
If you will be hosting a gathering during the holiday season that brings people who live in different households together, follow CDC tips for hosting gatherings. If you will be attending a gathering that someone else is hosting, follow CDC Considerations for Events and Gatherings. Below are some general considerations for hosting a gathering that brings together people from different households. Guests should be aware of these considerations and ask their host what mitigation measures will be in place during the gathering. Hosts should consider the following:
- Check the COVID-19 infection rates in areas where attendees live on state, local, territorial, or tribal health department websites. Based on the current status of the pandemic, consider if it is safe to hold or attend the gathering on the proposed date.
- Limit the number of attendees as much as possible to allow people from different households to remain at least 6 feet apart at all times. Guests should avoid direct contact, including handshakes and hugs, with others not from their household.
- Host outdoor rather than indoor gatherings as much as possible. Even outdoors, require guests to wear masks when not eating or drinking.
- Avoid holding gatherings in crowded, poorly ventilated spaces with persons who are not in your household.
- Increase ventilation by opening windows and doors to the extent that is safe and feasible based on the weather, or by placing central air and heating on continuous circulation.
- For additional information on increasing ventilation, visit CDC’s information on Cleaning and Disinfecting Your Home.
- Winter weather can be cold, wet, and unpredictable. Inclement weather makes it difficult to increase ventilation by opening windows or to hold an event outdoors.
- If setting up outdoor seating under a pop-up open air tent, ensure guests are still seated with physical distancing in mind. Enclosed 4-wall tents will have less air circulation than open air tents. If outdoor temperature or weather forces you to put up the tent sidewalls, consider leaving one or more sides open or rolling up the bottom 12” of each sidewall to enhance ventilation while still providing a wind break.
- Require guests to wear masks. At gatherings that include persons of different households, everyone should always wear a mask that covers both the mouth and nose, except when eating or drinking. It is also important to stay at least 6 feet away from people who are not in your household at all times.
- Encourage guests to avoid singing or shouting, especially indoors. Keep music levels down so people don’t have to shout or speak loudly to be heard.
- Encourage attendees to wash their hands often with soap and water for at least 20 seconds. If soap and water are not readily available, use hand sanitizer that contains at least 60% alcohol.
- Provide guests information about any COVID-19 safety guidelines and steps that will be in place at the gathering to prevent the spread of the virus.
- Provide and/or encourage attendees to bring supplies to help everyone to stay healthy. These include extra masks (do not share or swap with others), hand sanitizer that contains at least 60% alcohol, and tissues. Stock bathrooms with enough hand soap and single use towels.
- Limit contact with commonly touched surfaces or shared items such as serving utensils.
- Clean and disinfect commonly touched surfaces and any shared items between use when feasible. Use EPA-approved disinfectantsexternal icon.
- Use touchless garbage cans if available. Use gloves when removing garbage bags or handling and disposing of trash. Wash hands after removing gloves.
- Plan ahead and ask guests to avoid contact with people outside of their households for 14 days before the gathering.
- Treat pets as you would other human family members – do not let pets interact with people outside the household.
The more of these prevention measures that you put in place, the safer your gathering will be. No one measure is enough to prevent the spread of COVID-19.
Food and drinks at small holiday gatherings
Currently, there is no evidence to suggest that handling food or eating is associated with directly spreading COVID-19. It is possible that a person can get COVID-19 by touching a surface or object, including food, food packaging, or utensils that have the virus on it and then touching their own mouth, nose, or possibly their eyes. However, this is not thought to be the main way that the virus is spread. Remember, it is always important to follow food safety practices to reduce the risk of illness from common foodborne germs.
- Encourage guests to bring food and drinks for themselves and for members of their own household only; avoid potluck-style gatherings.
- Wear a mask while preparing food for or serving food to others who don’t live in your household.
- All attendees should have a plan for where to store their mask while eating and drinking. Keep it in a dry, breathable bag (like a paper or mesh fabric bag) to keep it clean between uses.
- Limit people going in and out of the areas where food is being prepared or handled, such as in the kitchen or around the grill, if possible.
- Have one person who is wearing a mask serve all the food so that multiple people are not handling the serving utensils.
- Use single-use options or identify one person to serve sharable items, like salad dressings, food containers, plates and utensils, and condiments.
- Make sure everyone washes their hands with soap and water for 20 seconds before and after preparing, serving, and eating food and after taking trash out. Use hand sanitizer that contains at least 60% alcohol if soap and water are not available.
- Designate a space for guests to wash hands after handling or eating food.
- Limit crowding in areas where food is served by having one person dispense food individually to plates, always keeping a minimum of a 6-foot distance from the person whom they are serving. Avoid crowded buffet and drink stations. Change and launder linen items (e.g., seating covers, tablecloths, linen napkins) immediately following the event.
- Offer no-touch trash cans for guests to easily throw away food items.
- Wash dishes in the dishwasher or with hot soapy water immediately following the gathering.
Travel and Overnight Stays
If you decide to travel, follow these safety measures during your trip to protect yourself and others from COVID-19:
- Wear a mask in public settings, like on public and mass transportation, at events and gatherings, and anywhere you will be around other people.
- Avoid close contact by staying at least 6 feet apart (about 2 arm lengths) from anyone who is not from your household.
- Wash your hands often with soap and water for at least 20 seconds or use hand sanitizer (with at least 60% alcohol).
- Avoid contact with anyone who is sick.
- Avoid touching your face mask, eyes, nose, and mouth.
Travel increases the chance of getting and spreading the virus that causes COVID-19. Staying home is the best way to protect yourself and others. Use information from the following webpages to decide whether to travel during the holidays:
- Travel During the COVID-19 Pandemic
- Know Your Travel Risk
- Know When to Delay Your Travel to Avoid Spreading COVID-19
- Considerations for traveling overnight
Considerations for staying overnight or hosting overnight guests
Consider whether you, someone you live with, or anyone you plan to visit with is at increased risk for severe illness from COVID-19, to determine whether to stay overnight in the same residence or to stay elsewhere.
- Assess risk for infection based on how you or your visitor will travel.
- Consider and prepare for what you will do if you, or someone else, becomes sick during the visit. What are the plans for isolation, medical care, basic care, and travel home?
Tips for staying overnight or hosting overnight guests
- Visitors should launder clothing and mask, and stow luggage away from common areas upon arrival.
- Wash hands with soap and water for at least 20 seconds, especially upon arrival.
- Wear masks while inside the house. Masks may be removed for eating, drinking, and sleeping, but individuals from different households should stay at least 6 feet away from each other at all times.
- Improve ventilation by opening windows and doors or by placing central air and heating on continuous circulation.
- Spend time together outdoors. Take a walk or sit outdoors at least 6 feet apart for interpersonal interactions.
- Avoid singing or shouting, especially indoors.
- Treat pets as you would other human family members – do not let pets interact with people outside the household.
- Monitor hosts and guests for symptoms of COVID-19 such as fever, cough, or shortness of breath.
- Hosts and guests should have a plan for what to do if someone becomes sick.
Gatherings can contribute to the spread of other infectious diseases. Getting a flu vaccine is an essential part of protecting your health and your family’s health this season. Flu vaccines are useful any time during the flu season and can often be accessed into January or later.
Steps to take if exposed to COVID-19 during a holiday gathering
If you are exposed to COVID-19 at a holiday gathering, while traveling, or at any time, quarantine yourself to protect others by doing the following:
- Stay home for 14 days after your last contact with a person who has COVID-19.
- Stay away from others, especially people who are at increased risk for severe illness from COVID-19.
- Watch for fever (100.4◦F or higher), cough, shortness of breath, or other symptoms of COVID-19
- Consider getting tested for COVID-19. Even if you test negative for COVID-19 or feel healthy, you should still stay home (quarantine) for 14 days after your last contact with a person who has COVID-19. This is because symptoms may appear 2 to 14 days after exposure to the virus, and some infected people never have symptoms but are still contagious.
- Do not travel until 14 days after your last possible exposure.
If you can’t completely stay away from others during the 14 days:
- Stay at least 6 feet (about 2 arm lengths) away from other people.
- Wear a mask that covers both the mouth and nose when you are outside of your home.
- Wash your hands often with soap and water for at least 20 seconds or use hand sanitizer that contains at least 60% alcohol).
- Monitor yourself and household members for symptoms of COVID-19.
- Get information about COVID-19 testing if you feel sick.
If you develop symptoms consistent with COVID-19 within 14 days of the event or celebration, such as fever, cough, or shortness of breath, or if you test positive for COVID-19, immediately notify the host and others who attended. They may need to inform other attendees about their possible exposure to the virus. Contact your health care provider and follow the CDC-recommended steps for what to do if you become sick, and follow the public health recommendations for community-related exposure.
If you have been diagnosed with COVID-19, a public health worker may contact you to check on your health and ask you who you have been in contact with and where you’ve spent time in order to identify and provide support to people (contacts) who may have been infected. Your information will be confidential. Learn more about what to expect with contact tracing.pdf icon
Holiday celebrations
Holiday celebrations will likely need to be different this year to prevent the spread of COVID-19. Avoid activities that are higher risk for spread. Consider fun alternatives that pose lower risk of spreading COVID-19.
Thanksgiving
Thanksgiving is a time when many families travel long distances to celebrate together. Travel increases the chance of getting and spreading the virus that causes COVID-19. Staying home is the best way to protect yourself and others. If you must travel, be informed of the risks involved.
- Having a small dinner with only people who live in your household
- Preparing traditional family recipes for family and neighbors, especially those at higher risk of severe illness from COVID-19, and delivering them in a way that doesn’t involve contact with others
- Having a virtual dinner and sharing recipes with friends and family
- Shopping online rather than in person on the day after Thanksgiving or the next Monday
- Watching sports events, parades, and movies from home
- Having a small outdoor dinner with family and friends who live in your community
- Lower your risk by following CDC’s recommendations on hosting gatherings or cook-outs.
- Visiting pumpkin patches or orchards where people use hand sanitizer before touching pumpkins or picking apples, wearing masks is encouraged or enforced, and people are able to maintain social distancing
- Attending a small outdoor sports events with safety precautions in place
Avoid these higher risk activities to help prevent the spread of the virus that causes COVID-19:
- Going shopping in crowded stores just before, on, or after Thanksgiving
- Participating or being a spectator at a crowded race
- Attending crowded parades
- Attending large indoor gatherings with people from outside of your household
- Using alcohol or drugs that may alter judgment and make it more difficult to practice COVID-19 safety measures.
- Stress and Coping
- Travel During the COVID-19 Pandemic
- Know Your Travel Risk
- Know When to Delay Your Travel to Avoid Spreading COVID-19
(To sign up for a free subscription to Food Safety News, click here.)
“As consumers are preparing more meals at home, it is important that these cooks are practicing food safety in their kitchens” says Mindy Brashears, USDA Under Secretary for Food Safety. “Our research shows that home cooks should read product labels to understand how to properly prepare an item, and not rely solely on appearance.”
Consumers may not know that some frozen foods are not fully cooked or ready to eat, especially if they have browned breading, grill marks or other signs that normally show that a product has been cooked. In a recent USDA study, 22 percent of participants said a not-ready-to-eat frozen chicken entrée was either cooked, partially cooked, or they weren’t sure that the product was in fact raw.
Frozen foods are convenient for busy families, because of how quickly they can be prepared. Frozen food products are also a great option because children can easily prepare frozen meals on their own. It is especially important for children to know how to practice the necessary food safety steps needed to prepare frozen meals to avoid foodborne illness, and to help them do so, parents must first understand if products are raw or ready-to-eat.
“Although some frozen products may look cooked, it is important to follow the same food safety guidelines as you would if you were cooking a fresh, raw product,” says Brashears. “Wash your hands before food preparation and after handling raw frozen products, and use a food thermometer to make sure your frozen meals reach a safe internal temperature.”
Among national survey respondents who had experience with foodborne illnesses, 61 percent reported they did not make changes to how they handled food at home after being sick, which is concerning when you consider that more than half of survey respondents reported that someone in their home was considered at-risk for foodborne illness. These individuals — children, older adults, pregnant women, and those with compromised immune systems — are unable to fight infection as effectively as others, so they can be susceptible to longer illness, hospitalization and even death from foodborne illness.
USDA shares the following recommendations to keep your family safe when preparing frozen meals.
- Inadequate handwashing is a contributing factor to all sorts of illness, including foodborne illness. It is important to follow proper handwashing steps before, during and after preparing frozen food to prevent germs from transferring from your hands to your meal.
- In this study, 97 percent of participants did not attempt to wash their hands during meal prep to prevent cross-contamination, which is consistent with results from previous observational studies.
- Of those who tried, 95 percent failed to wash their hands properly. There are five steps for proper handwashing: wet, lather with soap, scrub for 20 seconds, rinse and dry.
- Most participants failed to rub their hands with soap for a full 20 seconds.
- Although frozen products may appear to be pre-cooked or browned, they should be handled and prepared no differently than raw products and must be cooked. Frozen products may be labeled with phrases such as “Cook and Serve,” “Ready to Cook” and “Oven Ready” to indicate they must be cooked.
- Always use a food thermometer to check the internal temperature of your frozen meat and poultry products to determine whether they are safe to eat.
- Beef, pork, lamb and veal (steaks, roasts and chops): 145 degrees Fahrenheit with a three-minute rest time.
- Ground meats (beef, pork, lamb and veal): 160 degrees Fahrenheit
- Poultry (whole or ground): 165 degrees Fahrenheit.
- Frozen and raw produce may also carry germs that can cause foodborne illness. It is important to handle produce properly to prevent the spread of germs to your food and kitchen.
- When preparing the frozen corn for a salad, almost all participants in the study failed to follow the manufacturer’s instructions to check that it reached a safe internal temperature of 165 degrees Fahrenheit. A food thermometer is the only safe way to know if it reaches that temperature.
- Even if you are preparing a cold salad, frozen produce must be cooked first.
- If you are handling fresh produce, follow recommendations from the U.S. Food and Drug Administration (FDA) to rinse and scrub raw vegetables prior to peeling them. When preparing a cucumber for the salad, nearly half of participants rinsed and scrubbed the surface of the cucumber with their hands instead of using a vegetable brush while rinsing; FDA recommends using a brush for cucumbers and other hard vegetables.
- Check that frozen food in your freezer has not been recalled. You can find information about recalled items and how to handle them on the USDA and FDA websites.
- After learning about a recalled item, 94 percent of survey respondents who had the item in their home followed the recommendations from the recall: to discard the item or return it to the store.
- Consumers can visit FoodSafety.gov or the USDA’s FoodKeeper application to view all food recall information from USDA and the FDA.
The U.S. Centers for Disease Control and Prevention estimates that millions of Americans are sickened with foodborne illnesses each year, resulting in roughly 128,000 hospitalizations and 3,000 deaths. Follow these food safety recommendations to decrease the risk of foodborne illness in your home.
These findings are part of a multi-year, mixed-method study that FSIS commissioned to evaluate various consumer food handling behaviors. The study uses test kitchens, focus groups and nationally representative surveys to better understand food safety practices and experiences with food recalls, foodborne illness, and FSIS food safety resources. More information about this study is available in an executive summary.
(To sign up for a free subscription to Food Safety News, click here.)
]]>A new school year is approaching and with it, changes to your usual routine.
“Parents are juggling many decisions as students may be returning to school for the first time since the COVID-19 pandemic began, and others may still be distance learning,” said Mindy Brashears, Under Secretary for Food Safety at the U.S. Department of Agriculture (USDA).
“You don’t want to add foodborne illness – commonly called food poisoning – to your list of concerns, so take time to plan and prepare your children’s lunch meals safely.”
The USDA encourages families to be prepared by adding a few essential items to back-to-school shopping lists. They can be used to avoid mistakes in the kitchen that can lead to illness.
“Having the whole family follow some simple food safety behaviors can help them avoid all kinds of illnesses this time of year, including foodborne illness,” said Paul Kiecker, Administrator for USDA’s Food Safety and Inspection Service.
“This list of items can help you and your family make sure lunches and snacks are safely prepared, following the USDA’s four steps to food safety: Clean, Separate, Cook, and Chill.”
- Hand wipes, hand sanitizers, soap and towels — Now more than ever, it’s important to keep these items visible as a reminder to clean hands and surfaces. People tend to rush through the steps of washing when they are on-the-go. Recent USDA research conducted in test kitchens revealed participants were not washing their hands properly up to 99 percent of the time before and during meal preparation. Wash hands with clean, running water (warm or cold) and soap for at least 20 seconds and dry them with a clean cloth or towel. Hand wipes and 60 percent alcohol-based hand sanitizers can be used to clean hands and surfaces if water and soap are not available. Remember to wash cutting boards, dishes, utensils and countertops with soap and hot water after preparing each food item and before proceeding to the next item. A bleach-based solution can be used to sanitize surfaces and utensils.
- Different colored cutting boards — If you’re preparing perishable foods that require cutting (for example, bacon and chicken for salad) make sure you separate raw meat and poultry from ready-to-eat foods (such as fruits, vegetables, cheeses, etc.) to avoid cross-contamination. Harmful bacteria can spread throughout the kitchen and get onto cutting boards, utensils, countertops and other ready-to-eat foods you’re preparing. Different colored cutting boards are a good reminder of this step. Use a green cutting board for fresh produce and another color for meat and poultry.
- Food thermometers — A food thermometer is the only way to know that foods are safely cooked to a temperature high enough to kill any harmful bacteria that might be present. Have a food thermometer easily accessible. It will be easier to remember the cook step if the thermometer is always reachable.
- Insulated soft-sided lunch boxes,
gel packs, and appliance thermometers - — If children have lunch outside of the home, make sure they have an insulated, soft-sided lunch box or bag to keep perishable items in their lunch cold. A frozen gel pack, combined with a frozen juice box or bottle of water, should keep lunches chilled and safe until lunchtime. Place them on top and bottom of perishable food items to keep them cold and avoid the “Danger Zone” (temperatures between 40 and 140 degrees Fahrenheit where bacteria can multiply quickly and cause illness).
- Insulated containers — When children take a hot lunch outside of the home, insulated containers are important to keep food that should be served hot safe. Use an insulated container to keep soup, chili, and stew hot at 140 degrees Fahrenheit or above. Fill the container with boiling water, let it stand for a few minutes, empty, and then put in the piping hot food. Keep the insulated container closed until lunchtime to keep the contents hot.
Stop by the food preparation aisle at your grocery store to find many of these items on your back-to-school food safety list. By using them, you can keep your children — and the rest of your family — safe from foodborne illness.
Consumers can view some age-appropriate food safety lessons and learn more about key food safety practices at Foodsafety.gov, by following @USDAFoodSafety on Twitter and by liking Facebook.com/FoodSafety.gov. Consumers with questions about food safety can call the USDA Meat and Poultry Hotline at 1-888-MPHotline (1-888-674-6854) from 10 a.m. to 6 p.m. Eastern Time, Monday through Friday, in English or Spanish, or email to [email protected]. Consumers can also chat live at https://ask.usda.gov/.
(To sign up for a free subscription to Food Safety News, click here.)
]]>